While pregnant with my first baby, I did a lot of research into a hospital birth vs. a home birth. I already knew I wasn’t that comfortable with the hospital option (watch The Business of Being Born and you’ll see why I feel this way), but I was also hesitant about having a baby at home (and my husband was vehemently opposed to that idea). We didn’t realize until we started doing our homework that a third option was available to us: the Birth Center.
Choosing where to give birth is a major decision, and birth centers offer a supportive middle ground between hospital and home birth for many families.
What Is a Birth Center?
A birth center is a “home-like facility existing within a healthcare system with a program of care designed in the wellness model of pregnancy and birth” staffed by midwives, nurse-midwives, and/or obstetricians. Birth centers provide “family-centered care for healthy women before, during, and after a normal pregnancy, labor, and birth.”1
For my husband and me, the birth center was the middle ground we sought when it came to where I would have our baby. Since I was 100% against the hospital (unless necessary, of course) and he was 100% against home birth, when we discovered the birth center, we knew we’d found our solution for a natural, comfortable (as possible — I mean, it is labor after all!), and intervention-free labor and delivery experience. Here are some of the main reasons I chose to have a birth center birth for each of my babies.
1. Midwives vs. Doctors
Midwives often provide a more personal, continuous style of care, which many families prefer during pregnancy and labor.

In my experience, there is a stark difference in the level of care provided by a midwife versus that of an OB/GYN. In most cases, the OB/GYN is rushed and brief during most prenatal visits. He does the necessary check-up items for each prenatal visit while answering any questions you may have. The entirety of the visit lasts approximately 10-15 minutes (after you have waited around for your appointment to start for at least 30 minutes). At the main event, the OB/GYN often doesn’t even enter the room until you are crowning, so most of the hard work of coaching and supporting you is done by one or two nurses you’ve likely never met in your life.
On the other hand, midwives take far more time during your appointment to discuss any questions or concerns you may have. They also take the time to help you familiarize yourself with your baby and your body as it grows (my midwives helped me feel my baby through my belly to determine whether I was feeling a head or a bottom). During labor, the midwife is by your side the entire time. She is a coach, a mentor, and a friend. She guides you through the process and recognizes cues such as changes in breathing and/or moaning to help you understand what is happening to your body when it is happening. The midwife experience is a truly personalized and intimate experience that often develops into a lasting friendship.
Related: Midwife vs. OB/GYN: What’s the Difference and Who to Choose?
2. Cost
Birth centers are typically far less expensive than hospitals, especially for low-risk pregnancies.
There’s also a big difference in the cost of having a baby when you choose a birth center over a hospital. In most cases (and it always depends on whether your insurance will cover a birth center), having a baby at a birth center costs about a third of what it would cost to have a baby in a hospital.2 I had the unfortunate experience of paying for both with my first child since I spent 40 hours laboring at the birth center before transferring to the hospital, where I ended up delivering her. Seeing the difference between the bills from the birth center and those from the hospital was astounding.
3. More Autonomy
At a birth center, there is less pressure to consent to treatments you do not want for you or your soon-to-be-born child (more on this later). During the last weeks of your pregnancy, the midwife will sit down and talk to you about available treatments or procedures, such as APGAR testing. She will explain why each treatment is offered and address any questions you may have about it.
With a doctor, he would rarely sit down and discuss the pros and cons of these treatments; instead, they tell you what is typically done and all the good reasons for doing it, and encourage you to sign the papers for consent. I am the kind of person who needs to know ALL THE THINGS about a subject before I consent to it. I can’t just trust that it’s okay because it’s “the norm.” So being able to go over all the treatment options and have an educated discussion about each of them with my midwife was important to me.
Related: Birth Center Bag Checklist: What To Pack for Labor, Baby, and Postpartum
4. Fewer (Unnecessary) Medical Interventions
Birth centers focus on supporting the body’s natural process, which often means fewer routine interventions for healthy moms.

Giving birth at a hospital means you are more likely than not to be subject to numerous interventions, most of which are usually completely unnecessary for a healthy, low-risk pregnancy. According to the National Birth Center Study II, “Almost all women (87%) who labor in hospitals undergo continuous electronic fetal monitoring, 80% receive intravenous fluids, 47% have labor artificially accelerated with medications, and 43% of first-time moms have labor artificially induced.”3 Moreover, women who have their babies in a hospital have a four times greater chance of having a c-section.3 As stated in the study, “here is strong evidence that routine use of these practices, when carried out without medical indications, has few benefits and many potential harms for healthy mothers and babies.”3
None of these interventions are used at a birth center. Fetal monitoring is done by a handheld fetal doppler and is checked at regular intervals. There are no intravenous fluids, no medications, and no induction. Women are allowed to labor on their own time and in their own way.
One major benefit of laboring in a birth center is the ability of the mom to eat and drink during labor and to labor in any position she deems necessary (whereas in the hospital, 60% of women are not allowed to eat or drink, 76% are restricted to bed, and 92% give birth lying on their backs).3 Additionally, many birth centers offer laboring mothers the option of laboring and/or delivering their baby in the water, which many women have called the “natural epidural.”
Finally, for those moms who have chosen not to vaccinate their children or those who are still doing their research and haven’t made a firm decision, having a baby in a birth center allows the new family to choose whether or not to allow such interventions such as Erythromycin eye ointment, the vitamin K shot, vaccinations, and the heel prick test to their newborn. In a hospital, some of these interventions are required by law, while others are strongly encouraged, regardless of whether parents have had the opportunity to educate themselves on them.
5. All the Comforts of Home
Birth centers are designed to feel warm and home-like, helping laboring moms relax and move more freely.

Anyone who has ever visited or been admitted to the hospital knows how uncomfortable they can be. The beds are small and lumpy. Nurses are constantly going in and out of the room. You usually end up with needles in your hands and arms. The lighting is anything but soft, and the atmosphere is less than homey.
In a birth center, your room is similar to a bedroom. The bed is large and soft, usually with real sheets and fluffy pillows. The lighting is soft and low. Music is playing if you want it to be. And your midwife is the only one poking and prodding you, which is usually not very often. You can walk when you need to, eat when you need to, and labor in any position. If you’d like to take a shower, feel free to do so. If you want to labor in the warm tub, sink in. The entire goal of a birth center is to make you feel as comfortable as if you were in your own home.
One concern I often hear when discussing having a baby in a birth center is that the soon-to-be mom (and dad, too) are worried that if something were to happen, they wouldn’t be at a hospital with doctors, equipment, and medicine. I understand this concern, as my husband and I have had the same concern. Fortunately, most birth centers are very close to, if not already inside, a hospital.
For those birth centers that are not already in a hospital, a woman can be transferred to a hospital very quickly if she chooses to or if it is medically necessary. However, needing to be transferred to a hospital is a rare occurrence. According to the National Birth Center Study II, 84% of women who chose to give birth in a birth center actually gave birth there.3 Those women who transferred from a birth center to a hospital did so for non-emergency reasons (such as prolonged labor). Less than 1% of the women in the study were transferred for emergency reasons.3
I have experience with a transfer from a birth center to a hospital. As mentioned, I labored for 40 hours at a birth center with my first baby. I had gotten stuck at 7cm, and my baby was acynclitic (she was trying to come out with her head cocked to one side). Despite all of our best efforts to get her back in the correct position, she declined, being stubborn like her mama.
After so many hours of no sleep, little to eat, and a LOT of physical exertion and pain on my part, I chose to be transferred to the hospital simply so that I could get an epidural to achieve my goal of having my baby vaginally. By the time we got to the hospital, my sweet, stubborn girl had shifted her position, and I was at 9cm. A few hours later, she was indeed delivered vaginally, and she was healthy, fat, and happy. It was not the birth scenario I wanted for her or me, but it was what I needed to do at the time. And I am thankful that I could easily transfer to the hospital.
6. The Postpartum Experience
The hours after birth are precious, and birth centers often prioritize uninterrupted bonding and newborn care.
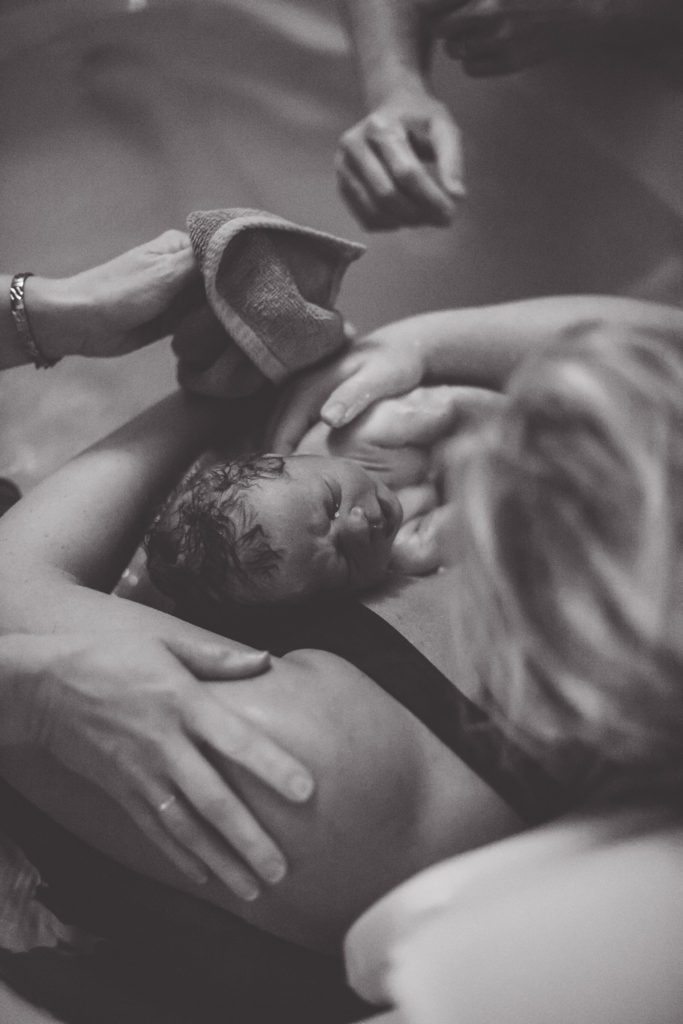
The minutes and hours after a baby is born are a crucial time for mother and baby to begin forming a strong bond. There are many things done in the hospital within those first critical minutes that can interrupt that important bonding time and physically impact the child’s health and well-being. In my experience (and I’ve experienced both settings), the postpartum experience in a birth center is light-years better than that of the hospital.
Related: The First 24 Hours of Baby’s Life: What To Expect
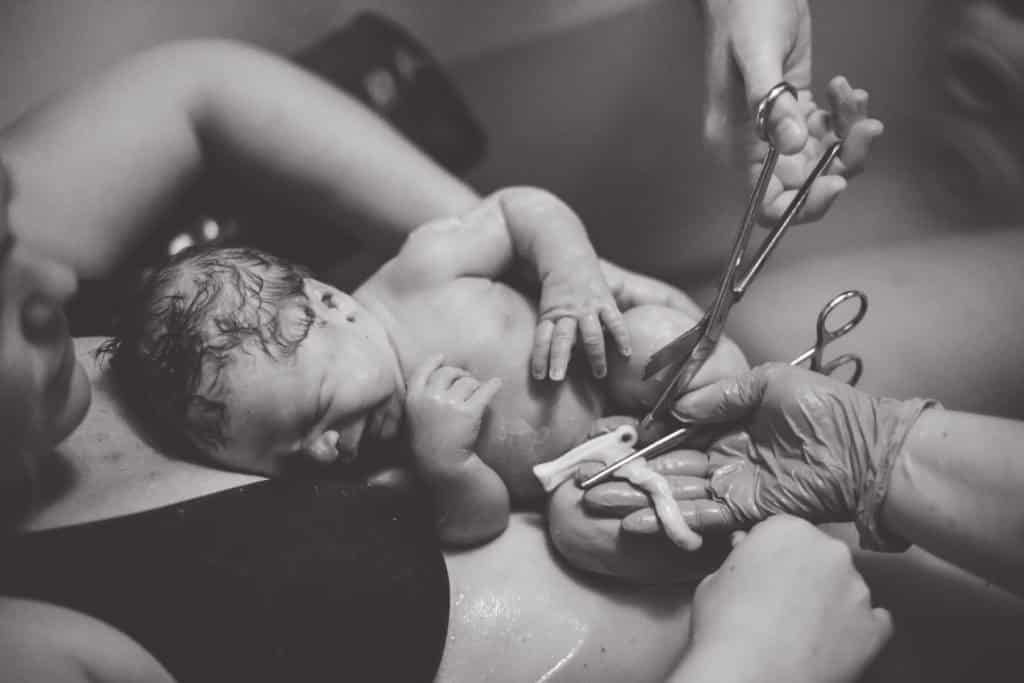
In the minutes after a baby is born in most hospitals (although many hospitals are moving toward being more baby-friendly these days), they immediately have their umbilical cord clamped and cut. They’re vigorously rubbed down with clean cloths and wrapped in a tight coil of blankets with their head covered in a knit hat. While this common practice may not seem so bad at first glance, there are several ways it can either disrupt the mother-child bonding experience or potentially negatively impact the baby’s optimal health.
First, delayed cord clamping is becoming the recommended standard over the more traditional method of clamping and cutting immediately.4 Delayed cord cutting offers many benefits to the baby, including higher birth weight, better early hemoglobin concentration, and increased iron reserves.4 While most professionals agree to let the cord pulsate for one to three minutes post-delivery, many midwives subscribe to the rule of cutting the cord only after it has stopped pulsing entirely, which could take much longer than 3 minutes.
Delaying the rub-down or bathing of a newly born baby is also better for the baby’s health than an immediate clean-up. The sticky, white coating of vernix that covers a newborn is excellent at protecting the newborn’s skin and helping it adapt to the outside world.5 It also helps stop water loss through the skin, aids in temperature regulation, and helps boost the child’s immunity. Vernix protects the newborn for as long as it remains on the skin. By rubbing the vernix off the baby’s skin as soon as he is born, the baby loses many of its incredible benefits.5 Delaying the cleaning and/or washing of the baby’s skin for as long as possible will do the child a world of good.
Related: Why You Shouldn’t Give Your Baby a Bath Immediately After Birth
Additionally, wrapping the baby tightly in blankets before handing it to the mother interrupts the very important act of “kangaroo care,” or skin-to-skin time.6 Kangaroo care is a method of holding a baby, naked or with only a diaper, against the bare chest of a parent, usually the mother, for an extended period of time. The benefits of kangaroo care for a baby include a stabilized heart rate and breathing, improved oxygen saturation, rapid weight gain, more restful periods of sleep, and decreased crying, among other benefits.6 If done right after the birth, kangaroo care offers the added benefit of encouraging immediate breastfeeding.6
Finally, one benefit of using a birth center over a hospital that many people overlook is the postpartum support that midwives offer new mothers, which OB/GYNs do not or cannot offer.7 After the birth of my first child, as I started experiencing symptoms of postpartum depression, I mentioned my symptoms to the doctor who delivered my daughter at my 6-week postpartum check-up. He readily admitted that he was not as well educated or equipped to diagnose and treat postpartum depression. He suggested I go to my general doctor or a psychiatrist for further diagnosis. As disappointed as I was to hear this, I appreciated his honesty, and I went to my midwife to ask for her advice.
Related: How to Recognize and Treat Baby Blues vs Postpartum Depression
My midwife offered me the resources I needed to help find a solution to my postpartum depression. We tried many natural methods that often work for many women. However, in the end, we agreed that I needed to see my general practitioner for a prescription for antidepressants. My midwife also offered invaluable insight and advice when I had issues breastfeeding and connected me with a fantastic lactation consultant who could further help me.
While hospital birth is still the norm for women in the U.S., that does not always make it the best choice. Alternative options, such as home birth or birth centers, are steadily becoming more widely known and available choices. Moms and their significant others need to research the pros and cons of each available option so that they may make an educated and informed decision. The birth of a baby is an exciting yet stressful time. Being comfortable deciding where to have your birth experience helps to take some of that stress away so that you can better enjoy the crazy, incredible journey.
Above all, trust yourself as you explore your birth options and choose the setting that feels right and safe for your growing family.