Julie was excited and nervous during her first pregnancy. It took years of trying, miscarriages, consultations with fertility specialists, and rounds of in vitro fertilization to finally conceive. When she eventually became pregnant, Julie was hesitant to celebrate wholeheartedly. She wanted to see her son, hear his cry, and hold him before believing she would finally be a mom.
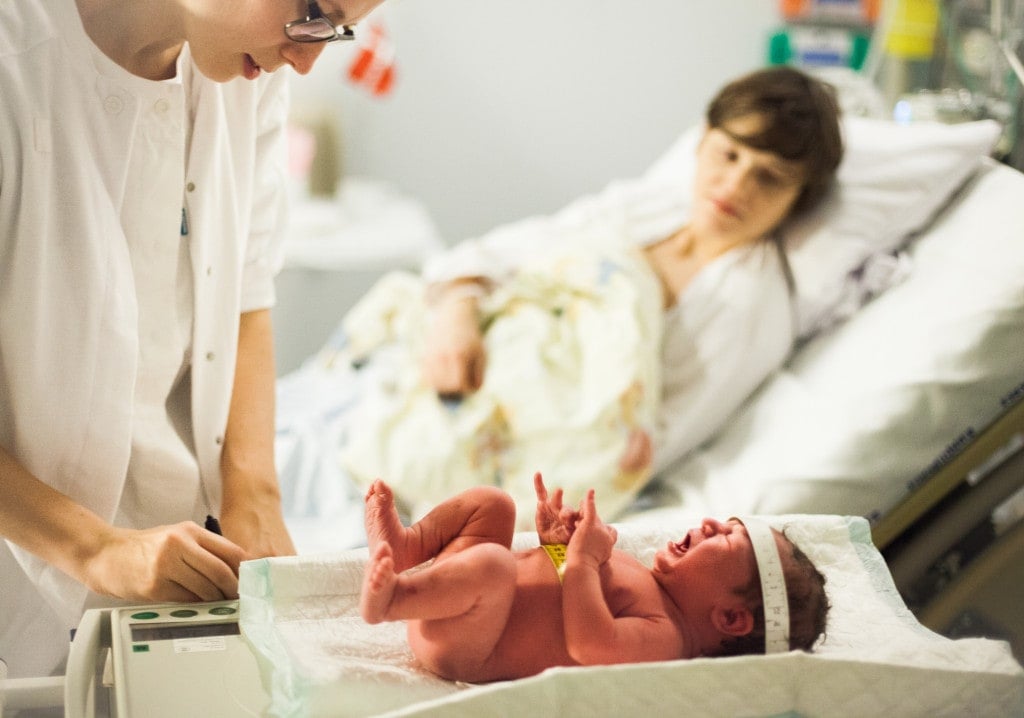
The day of Julie’s delivery was surprising. Her water broke unexpectedly three weeks early, and she arrived at the hospital already dilated. When the baby’s heart rate was irregular, the doctors decided to do an emergency C-section. The baby was born, and the operating room was filled with hustling nurses, resuscitation measures, and medical jargon. Julie could see her baby in the distance, but her tears blurred her vision.
“APGARs are 6 at one minute and 8 at five minutes,” she heard the doctor say to a nurse.
Julie didn’t know what that meant. Was that good? Or bad? What did those numbers mean?
Finally, after what felt like an eternity, Julie heard her baby crying for the first time. The doctor brought her beautiful baby boy to her, and she could kiss him for the first time.
If Julie’s story sounds familiar, it is because it is common. No two pregnancy and birth stories are alike. But parents find both individuality and commonality in their parenting journeys. One common thing across most birth stories is the assignment of APGAR scores to babies immediately after delivery.
What Is an APGAR Score?
The APGAR score was invented by Dr. Virginia Apgar, an anesthesiologist at New York-Presbyterian Hospital, in 1952 to assess a baby after birth.1 Later, doctors and medical staff followed up on her method and developed the acronym “APGAR” to determine a baby’s Appearance, Pulse, Grimace, Activity, and Respiration. A doctor or midwife will score these things after birth to determine if the baby needs medical intervention. The APGAR score continues to be widely used in hospitals by health care providers worldwide.
The APGAR “test” (or assessment) is typically done twice: first at 1 minute and then 5 minutes after birth. It may also be repeated later, depending on the situation. Generally, the APGAR scores inform healthcare providers how well the baby has transitioned from life inside the womb to life outside the womb.
How Is the Score Calculated?
Health care providers will evaluate the newborn baby on five simple criteria on a scale from 0-1-2, then sum up the five values. The resulting final score will range from 0 to 10. The criteria are:
- Breathing effort
- Heart rate
- Muscle tone
- Reflexes
- Skin color
As mentioned, each category is scored with 0, 1, or 2 at the 1-minute mark and then at 5 minutes, depending on the observed condition of the baby. The baby will then get a score on a scale of 1 to 10.
What Does the APGAR Score Mean?
For health care providers, the APGAR score is done to determine whether a newborn needs help breathing or is having trouble after birth. The 1-minute score defines how well the baby tolerated the birthing process. The 5-minute score tells the doctor how well the baby is doing outside the mother’s womb. The higher the score, the better the baby is doing after birth. For example, if a baby is struggling to breathe one minute after being born, he may receive an initial score of 1 for his breathing, and then once his breathing improves after 5 minutes, this score may go up to 2.
A score of 7, 8, or 9 out of 10 is considered reassuring and signifies that the newborn is in good health and is transitioning successfully. It is important to note that a score of 10 is very unusual since almost all newborns experience blue hands and feet. This is normal after birth, but it may also mean they lose 1 point.
A score of 6 and below is generally regarded as low and could result in immediate efforts to resuscitate the baby in the delivery room. Reasons for a low 1-minute score could include a long or difficult birth, fluid in the baby’s airway, or heart problems. A baby with a low APGAR score may need oxygen and clearing of the airway to help with breathing or physical stimulation to get the heart beating at a healthy rate. A low score on the 1-minute mark does not necessarily indicate a long-term problem, particularly if the score improves at the 5-minute mark. Most of the time, a low score at 1 minute is near-normal by 5 minutes. Once this score has normalized, the remainder of the postpartum period is typically routine and standard.
What Does the Score NOT Mean?
The APGAR score is neither a competition nor a badge of honor. After the neonatal period, the APGAR score is no longer relevant to a baby’s well-being. Whether a baby has a high or low score at birth typically has no predictive value for the future. Once the postpartum period is over, regular physical exams and wellness check-ups take over routine infant care. It cannot be emphasized enough that a lower APGAR score does not mean a child will have serious or long-term health problems. The score is explicitly used to inform healthcare providers of the baby’s needs post-delivery, if any.
In summary, the APGAR test determines quickly whether or not a newborn needs immediate medical care or further resuscitation. It is not designed to predict long-term health issues. In the case of Julie and her newborn baby Jett, although he had a “low” APGAR score at 1 minute, his 5-minute score was “normal” and reassuring to the health care providers. He required a little stimulation and suctioning and then was placed skin-to-skin with his mom.
Julie could then move on to the next chapter of her life: parenthood.