Perineal tearing is one of the most common concerns expectant parents have when preparing for a vaginal birth. While tears are common, there are ways to help reduce your risk and support healing afterward.
As a pelvic floor physical therapist, I regularly work with postpartum patients recovering from perineal tears. I’ve seen firsthand how proper preparation, recovery, and rehabilitation can make a significant difference in comfort and long-term pelvic health.
Here’s what to know about perineal tearing, including what causes it, how to reduce your risk, and what recovery may look like if it happens.
Key Takeaways
- Perineal tears are common during vaginal birth.
- Most tears are mild and heal well with proper care.
- Perineal massage may help reduce the risk of tearing.
- Birth position and pushing techniques can influence tearing risk.
- Pelvic floor rehabilitation can support recovery after birth.
What Is Perineal Tearing?
The pelvic floor muscles and vagina can stretch to more than three times their normal size during vaginal birth.4 The nerves that allow these muscles to move are stretched up to 35%.5 Under normal conditions, this would always result in injury; however, the hormonal shifts during pregnancy allow a birthing person’s skin and muscles to be stretched much more than normal.6,7
During vaginal birth, the area at the bottom of the vagina can tear. Tearing can occur in the vagina, vulva, perineum, or the area between the vagina and anus or into the anal sphincter. A tear can be as limited as the skin of the vaginal opening or as deep as the anal sphincter.8,9
Tears are graded from the first to the fourth degree.8 A first-degree tear only includes the skin and mucosa.8,10 A second-degree tear extends into the muscles.8
First- and second-degree tears generally aren’t related to leakage of the bowels or bladder.11,12 Third- and fourth-degree tears extend into muscles and anal sphincters and need surgical repair.8 Having a third- or fourth-degree tear may predispose you to leaking stool later, making rehabilitation even more important.11,12
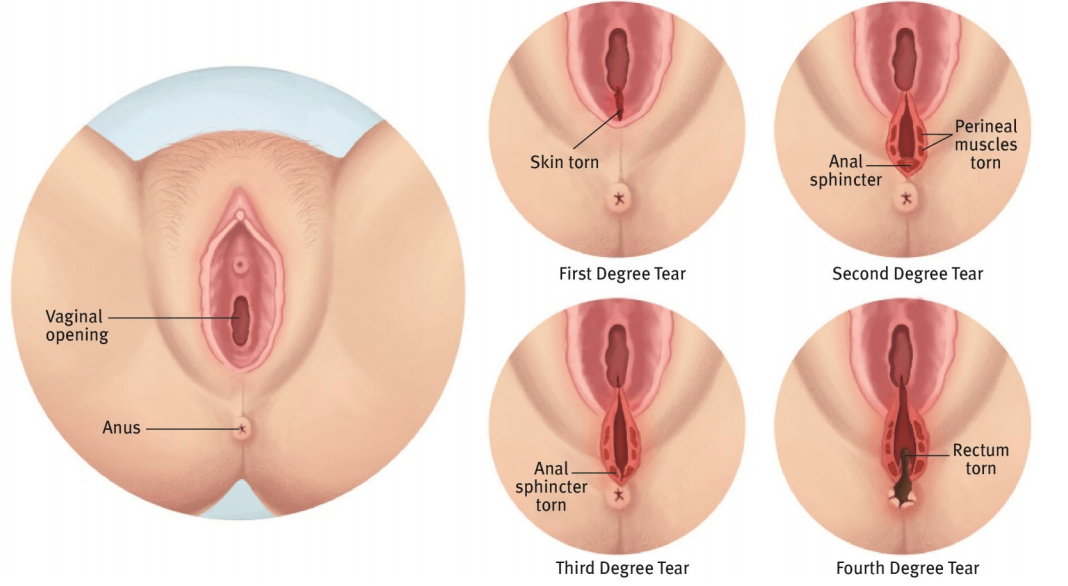
Related: Degrees of Perineal Tearing in Childbirth
How Common Are Perineal Tears?
Understanding how common tearing is can help set realistic expectations for birth and recovery. According to the American Urogynecologic Society, tears occur in up to 90% of women during their first birth and between 44% and 79% of birthing women overall.1 Tears are related to the baby’s size (whether or not it’s your first delivery), situational factors during birth, and your genetics.8,13
What Does a Tear Mean?
The severity of a tear can affect both short-term recovery and long-term pelvic floor function. Any injury must form scar tissue to heal, which takes 6 to 8 weeks.14 Yet scars are weaker than normal tissue and can cause pain and contribute to pain with sex and urinary or fecal incontinence.15
Additionally, in the early days of postpartum, tears can make peeing and pooping after birth much more uncomfortable.16 Luckily, there are ways to help ease that first time on the toilet, such as using a peri-bottle.8
Related: How to Prepare for Your First Poop After Birth
Can You Prevent Perineal Tearing?
While there is no guaranteed way to prevent perineal tearing, certain strategies may help reduce your risk and support healthier tissue during birth.
4 Tips To Minimize Your Risk of Tearing
Several factors can influence whether tearing occurs during birth. While some are outside your control, these are the strategies I most often recommend to patients who want to prepare their bodies for labor and delivery.
1. Do Perineal Massage
Starting to massage the perineum between 34 and 36 weeks can help the tissues stretch better.2 Research shows that it doesn’t cause any harm and may help reduce your risk of tearing.3 You can follow these steps to massage your perineum:
- Start by applying a warm, wet washcloth to your perineum or taking a warm bath.
- Ensure you have clean hands and trimmed nails. Lay reclined and use a mirror if you would like.
- Apply lubricant to your fingers. Make sure it’s a good lubricant, free of parabens and glycerin.17
- Insert one or two thumbs about 0.5 to 1 inch.
- Apply gentle pressure down and out diagonally for one to two minutes. Then press straight down for 1 to 2 minutes. Use your fingers to make a “U” shape or a smiley face.
- Perform this a few times per week for three to five minutes.
Related: Perineal Massage: What Is It and How To Do It?
2. Learn How To Push Correctly
When you go into the pushing stage, you use your diaphragm, abdominals, and pelvic floor to help with birthing.18 Your pelvic floor muscles have to open while your abdominal muscles and diaphragm create pressure from above to help your uterus push out your baby. Learning how to relax your pelvic floor and push correctly can help you open better during birth.
The pelvic floor muscles interact with our breathing muscles, and it’s important to make sure they’re working together well.18 Practicing deep diaphragmatic breathing can be helpful for pelvic floor relaxation as well.19 Everyone asks me about Kegels, but pelvic floor relaxation is key during labor and delivery! And knowing when to push is just as important as how to push.
Related: How to Push During Childbirth: Positions and Tips That Help
3. Consider Your Positioning During Birth
Your position during birth can increase or decrease your risk for tearing and pelvic floor muscle injury.10,13 For example, lying on your side or getting onto your hands and knees reduces damage to the pelvic floor.20,21 If you choose an epidural, lying on your side with a partner or sling lifting your leg is a great option.22
On the flip side, lying on your back can restrict the motion of your tailbone and is related to a higher rate of perineal tears. Squatting also leads to a large number of tears.22 In the United States, we don’t squat often enough to make it a natural birth position. In other cultures, people squat regularly (to have a conversation, eat, and empty their bladder).23
4. Build a Great Team
Choose birthing professionals who will respect your wishes about positioning and pushing. If you have a doula, they can help reduce the likelihood of a C-section and having an operative birth. Ask your midwife or physician whether they’re comfortable supporting different labor and birth positions.
Related: What Is a Doula? What They Do and the Benefits of Having One
So You Tore, Now What?
My advice to most pregnant people is to prepare for a perineal tear and healing because, statistically, it will happen. In the short term, make sure you have a pain management plan. Typical pain management can include having ice packs, sitz baths, medications, and padsicles, and preventing constipation.8
Also, prepare yourself for your first poop and pee. The first time you go can be painful, even if you didn’t suffer a tear.24,25 Here are some tips if you do tear:
Prepare for the Long Term
Once healing has taken place, think about retraining your pelvic floor muscles and core. Regardless of how you gave birth, the pelvic floor and abdominal muscles were distended by your growing uterus and need rehabilitation.26 In France, all birthing people see a pelvic floor therapist, which I’d love to see catch on in the U.S.27
If you have any scars from giving birth vaginally or via C-section, you can massage the scars by yourself or with the help of a professional or partner.15 Scars take six to eight weeks to close and about 12 weeks to finish healing.14,28 After the scar heals, massaging it directly can help the tissue remodel so the haphazard and weak collagen of scar tissue is broken down and strengthened.14
Scar tissue is often uncomfortable and may cause negative emotions. Scars can affect how much you leak and lead to pain with sex.8,15 Some people need to start very gently with a warm washcloth in the shower. Remember, nerves take longer to heal than skin and muscle. Any superficial skin nerves that were cut or torn through may feel like tingling, burning, or pain.
Disclaimer: This does not constitute or replace medical advice or evaluation.
Related: Perineal Care Postpartum: Tips for Healing After Birth
Find a Pelvic Floor Physical Therapist
If you’re experiencing ongoing pain, leakage, scar discomfort, or concerns about recovery, a pelvic floor physical therapist can help assess your symptoms and guide treatment. Here are some online resources for finding a pelvic floor physical therapist near you:
Watch: Reducing Your Risk of Perineal Tearing During Birth
I recently spoke with Dr. Julianna Allen about ways to help reduce the risk of perineal tearing during birth.
The Bottom Line
Perineal tearing is common, but it doesn’t have to be something you fear. Preparing your body for birth, understanding your options during labor, and prioritizing recovery afterward can all help support healing and long-term pelvic health. And if you do experience a tear, remember that support and treatment are available.