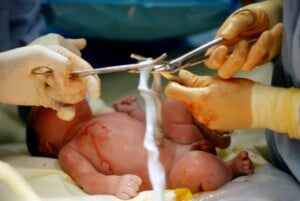
My birth plan was all typed out and edited. I’d read everything I could about the pros and cons of typical birth procedures. I wanted skin-to-skin contact as soon as possible, I wanted my partner to clip the cord after it stopped pulsing, and I did not want a routine episiotomy.
The contractions started so close together that there was no waiting time. The nurses did not believe they were as close as I was reporting. My partner and I were trying to play cards on the bed, but I was feeling worried. Every two minutes, like clockwork, another contraction waved over me. “Go for a walk, dear. It will be a while yet,” a nurse told me without any physical check. I got up and tried to go for a walk, but a single, very sharp contraction stopped me. Then I went to the washroom and got sick. I knew I was in transition labor.
As I was on the bed, ready to push, an elderly doctor entered the room. He walked up to me, picked up a scalpel, and immediately sliced a small incision in my perineum. At the time, it didn’t seem relevant. I was about to become a mother! In only two pushes and a total of two hours of labor from the first contraction, I was holding my baby. Nothing else mattered; not even my well-crafted birth plan or the raw pain I felt meant a thing. He was here, and he was perfect.
Luckily, my healing process was minimal and did not result in any further complications. However, many other women are not so fortunate.
The Tenuous History of Episiotomies
Episiotomies were first recommended in 1714 as a method of preventing severe tears to the perineum. The popularity of this procedure spread over the world. Even though it is one of the most common surgical procedures performed worldwide, solid research has never backed the efficacy of episiotomies.1
The idea behind episiotomies is that they help prevent fissures and provide a more safe and efficient delivery. Episiotomies are typically recommended for complications such as a breech delivery.1 However, many clinicians began performing routine episiotomies with the belief that they prevent more severe tearing. This thinking is flawed from the start since performing routine episiotomy guarantees that trauma (and resulting sutures), rather than leaving it to happen naturally, if at all. More recently, several studies have shown that routine episiotomies performed with the belief that they will reduce vaginal trauma are not justified.2
The World Health Organization (WHO) agrees and has suggested that episiotomies should not be a routine practice. Even more striking, the WHO says a woman’s informed consent is essential before performing an episiotomy.3 In 2006, the American College of Obstetricians and Gynecologists also recommended against performing routine episiotomies, stating that they do nothing to benefit the mother or the baby.4
In 1979, 60.9% of all vaginal deliveries in the United States had an episiotomy performed. By 2004, that rate had decreased to 24.5%. However, there is no apparent optimal rate of episiotomy.1 Much of the decision-making is still up to the doctor in charge.
Why Episiotomies Are More Hurtful Than Helpful
Take a piece of paper and make a small cut with some scissors, then pull the two sides of the paper. How easily did it tear? Now, try the same thing with a piece of paper you haven’t cut. Which piece of paper was the easiest to tear? Episiotomies work similarly. Cutting into the vaginal wall can indeed result in the opposite desired effect of preventing a tear and, instead, increase the risks of more traumatic tears.8
Tearing is a natural and common part of the childbirth process. Upwards of 79% of women who have vaginal births end up with tearing, most of which are minimal and don’t need stitches as they can heal perfectly well without any intervention. More severe tears are less common but can cause lasting issues and require stitches.8
As with the piece of paper, episiotomies can intensify the risk of more severe tears. Worse, tearing along the incision line can occur even during a natural delivery that would otherwise have only resulted in a slight, easily managed tear — or none at all.8,9
Are Episiotomies Ever Necessary?
Even though episiotomies are much less effective than previously thought, there are still some instances when they might be ideal. For example, if a mother is pushing and the fetal heart rate drops too low, an episiotomy may be performed in hopes of speeding up the delivery process. If the baby has broad shoulders and becomes stuck in the birth canal, an episiotomy may create some more room for the baby to emerge. Studies have shown that episiotomy rates at hospitals adopting these guidelines for unnecessary episiotomies have dropped dramatically.5
According to one safety organization, the ideal rate of episiotomy is about 5%.7,10 However, some hospitals have been able to reduce this rate to less than 3% when following specific guidelines for performing episiotomies only when necessary.7
How To Avoid an Episiotomy
One of the first things you can do is discuss routine episiotomy with your doctor. Depending on where you live, you may or may not have that same doctor with you in the delivery room. Looking into your hospital’s episiotomy rate can also provide you with some insight. Check with the hospital policies on how they reduce episiotomy rates and what other options they have in place.
Although my birth plan didn’t help me, it could help you. It’s still worth writing it out, even if you get sideways glances from a midwife or care provider who is much more in tune with current recommendations.
To reduce your risk of tearing during delivery, you can try perineal massage, applying warm compresses before and during labor, or giving birth in the water. All these reduce the tension and pressure on the perineum during delivery. Perineal massage has been studied extensively and is shown to help relax the tissues, reducing the likelihood of tearing.6
We Still Need Progress
Unfortunately, although rates are declining, episiotomies are still performed at higher rates than the recommended amount by many hospitals and doctors.11 By the time I had my episiotomy, they had been discouraged for some time.
When I went to meet my midwife for a checkup during my pregnancy with my daughter, I explained to her that I wished not to have a routine episiotomy. She looked at me with a mixture of shock and confusion and said, “Routine episiotomies haven’t been performed for years — at least a decade.”
It was clear to me that the doctor who performed my routine episiotomy was one of these older gentlemen still stuck in the ’70s performing them at will for no other reason than it was what he was used to. Speak up if you are concerned about the risk of unnecessary episiotomy. Women are at the forefront of change, and our voices are being heard.7