It’s the moment parents dread and pray never happens to them: Your baby is ill or injured. Every child will get hurt at some point. They fall, get burns, or eat something they shouldn’t. While we do our best to protect our children, the most important thing a parent can do is learn first aid for babies and what to do in common emergencies.
Nearly every parent has a moment of terror when their child hurts or is sick. However, having knowledge and foresight can help you not panic. You can also try to calm your child and prevent them from panicking. First, it is crucial to determine whether your child is experiencing a true emergency and proceed quickly and intentionally. Below are everyday emergencies and what to do in each one.
Note: If you are currently in a life-threatening emergency, stop reading and call 911 immediately, as this article is for informational purposes only.
Unconsciousness
If your baby is unconscious, but you do not know what happened, you should first assess the scene for the baby’s and your safety. If the location is safe, try to rouse your baby. Yell their name and stroke or tap the bottom of their feet. While doing this, assess whether they are breathing, if they are bleeding, or if there is some other apparent life-threatening condition. Do not spend more than 10 seconds trying to get their attention and assessing them.

Compressions and Breaths
If your baby does not respond, call 911 and get equipment and help if available. Place the baby on its back on a flat, firm surface like the floor. Begin compressions at a rate of 100-120 beats per minute.1 You can wrap your hands around the infant’s chest, using your thumbs or two fingers parallel to the chest for infant compressions. Your compressions should be about 1 ½ inches deep and allow full chest return after each compression. For older children, you can use the heel of one or both hands for compressions and should go closer to 2 inches in depth.
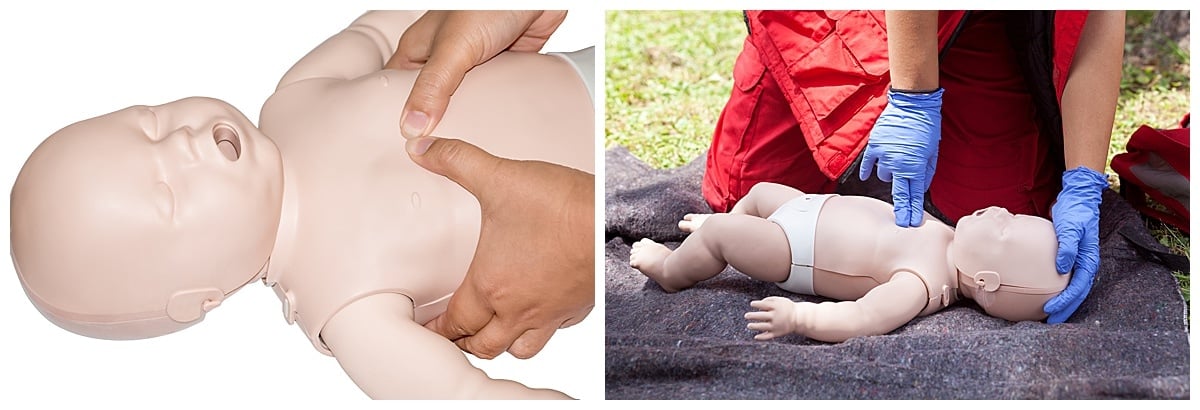
Count your compressions aloud, and when you have reached 30 compressions, give two breaths. Tilt the infant’s head back and lift their chin, blowing into their mouth for one second. Make sure that your breaths are causing the baby’s chest to rise. After two breaths, return to compressions. Alternate 30 compressions with two breaths until the infant resumes consciousness or help arrives. If you are alone and have been doing CPR for more than two minutes, or five sets of 30 compressions and two breaths, call 911 if you haven’t already.
The thought of doing CPR can be intimidating, even to a trained professional. Still, CPR can double or triple a person’s chances of survival if started within the first few minutes of cardiac arrest. It is important to note that you do not need formal training or certification to perform CPR. All you need is education and confidence. As silly as it may seem, you should practice CPR in a low-stress, non-emergent situation to prepare for emergencies.
Head Injury
Falls and injuries are unavoidable as babies learn to sit, walk, and move. Keeping an eye on them and ensuring their environments are safe can help, but here is what to look for and what to do to provide first aid for babies if they have a head injury:3
If your baby is unconscious or unresponsive following a head injury, do not move them in case of a neck or spine injury. If the child is vomiting or convulsing, roll them onto their side to prevent choking but maintain their head and neck in alignment. Call 911.
Call your pediatrician immediately if your baby experiences any loss of consciousness, difficulty waking or consoling, abnormal walking or talking, or multiple episodes of vomiting. You should also call your provider if your newborn baby has a head injury.
If your baby’s head injury is mild based on the criteria above, apply ice wrapped in a cloth to the injured area for 20 minutes every three to four hours. Closely observe your child for the 24 hours immediately following the injury, looking out for abnormal skin color, or breathing patterns. You do not need to keep your child awake after a head injury, but if your child naps or goes to bed shortly after the trauma, it is a good idea to check on them while they are sleeping.
Always trust your instincts if you think something is off with your child. Calling the pediatrician is a good idea if they are not looking or acting right.
Choking
Choking occurs when your baby cannot breathe because food or a foreign object is blocking their throat or airway. Keep small toys, buttons, and balloons away from babies and toddlers. Always serve babies food cut in a developmentally appropriate shape and size. Avoid offering whole grapes, nuts, and popcorn until age 4. However, even the most cautious parents can find themselves in a situation where their child is experiencing a choking episode.
Signs of Choking
Signs of actual choking include blue skin, difficulty breathing, unresponsiveness, inability to cry or cough, or soft, high-pitched sounds while inhaling, called stridor.4 Strong coughs, gagging, or crying are not signs of actual choking and can help the child dislodge the object. Here is how to recognize and provide first aid to babies when choking:
If your infant is choking, place them face down on one forearm with their chin in your palm. Angle their head slightly down toward the floor. You can do this from a seated position, using your lap to support your arm. With your free hand, deliver five strong back blows between their shoulder blades.

If the object is still stuck, flip the child over, keeping them on your forearm, and deliver five chest thrusts. Use two fingers from your free hand to compress their chest on their breastbone, centrally located just below the nipples. Compressions should go one-third to one-half of the chest’s depth.
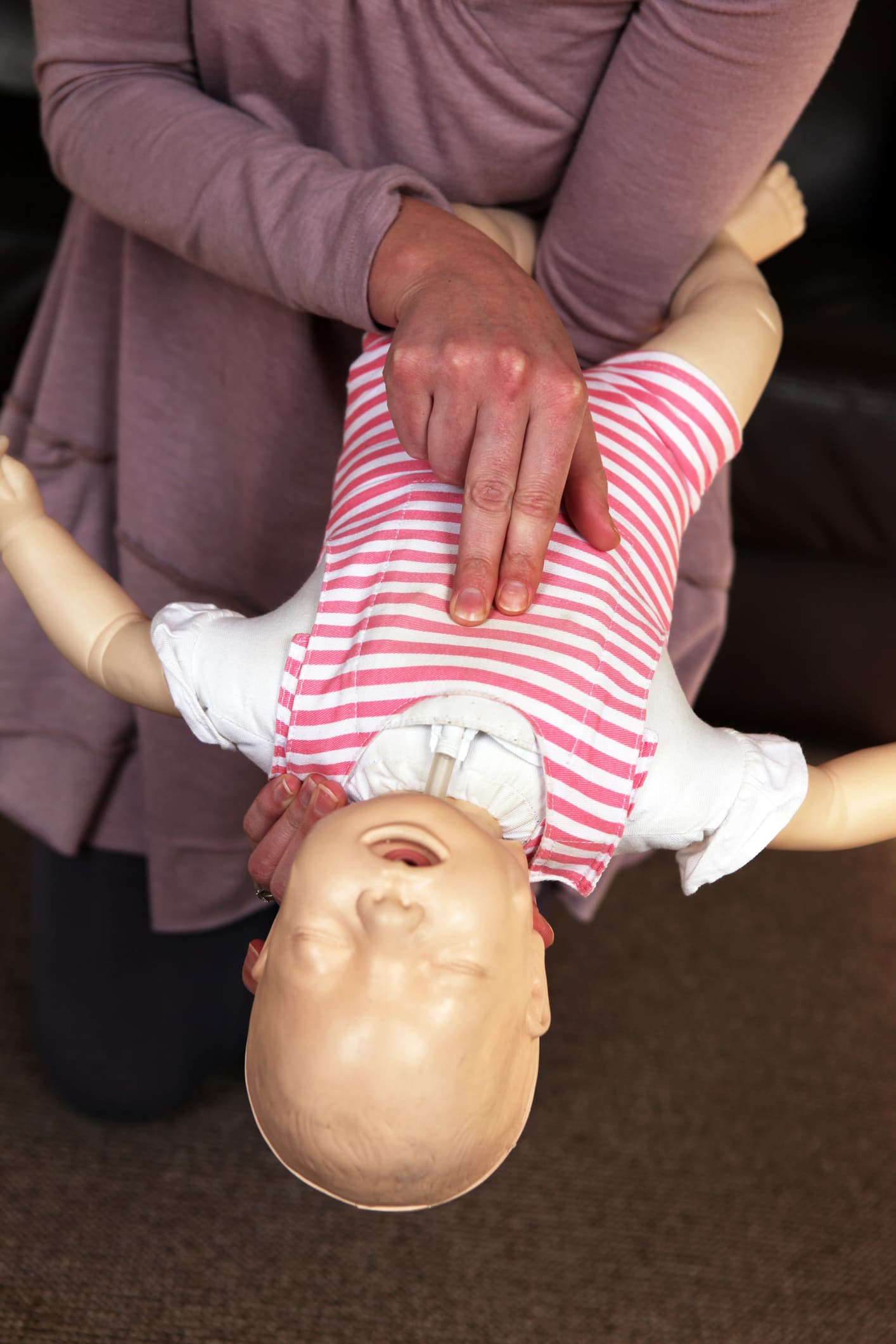
Alternate five back blows with five chest thrusts until the object dislodges or the infant becomes unresponsive. If the infant loses consciousness, shout for help, call 911, and begin CPR. If you can see the object, it is okay to try to remove it with your fingers, but never do a “blind sweep,” as this may further wedge the object, and never try to remove the object if the child is conscious.5
Wounds
Treatment of wounds when it comes to first aid for babies depends on the type and source of the wound. For instance, some wounds may require treatment with a tetanus booster or a course of antibiotics. Reaching out to your pediatrician for any wound is never a bad idea.
Abrasions

Abrasions are superficial scrapes on the top layer of skin. They are typically mild and do not cause much blood loss but are a common minor emergency. However, cleaning the area gently with soap and water is still essential. Failure to do so can cause an infection or scarring. Cover the abrasion with a clean, dry bandage, but be aware that bandages can be a choking hazard in infants. Keep the area clean and dry, and monitor for signs of infection, such as warmth, redness, swelling, or drainage at the site. Unless the abrasion covers a large body area, is located near the eye or on the face, or is embedded with debris, there is usually no need to call the pediatrician.6
Puncture Wounds

A puncture wound is when a sharp object penetrates deeply into the skin, such as a nail or a piece of wood or metal. Although the injury may be narrow, the depth of the wound makes it particularly susceptible to infection because bacteria and other germs are carried deep into the body tissue.
If the object that caused the puncture is still embedded in the skin, it is usually best to have it removed by a doctor. To provide first aid for babies at home, you can apply pressure for at least 5-10 minutes with a clean, dry cloth if there is no object in the skin. If the cloth becomes saturated, you should add another but do not remove the original one, as it is essential to maintain pressure to control bleeding.
Gently wash the wound with soap and water once the bleeding stops to ensure all residue and debris are rinsed away. Apply a bandage and call your child’s doctor. Calling 911 or visiting the emergency room is appropriate if the bleeding is profuse and not stopping. Be sure to keep the area clean and dry and avoid reinjury to the wound while it heals.7
Lacerations
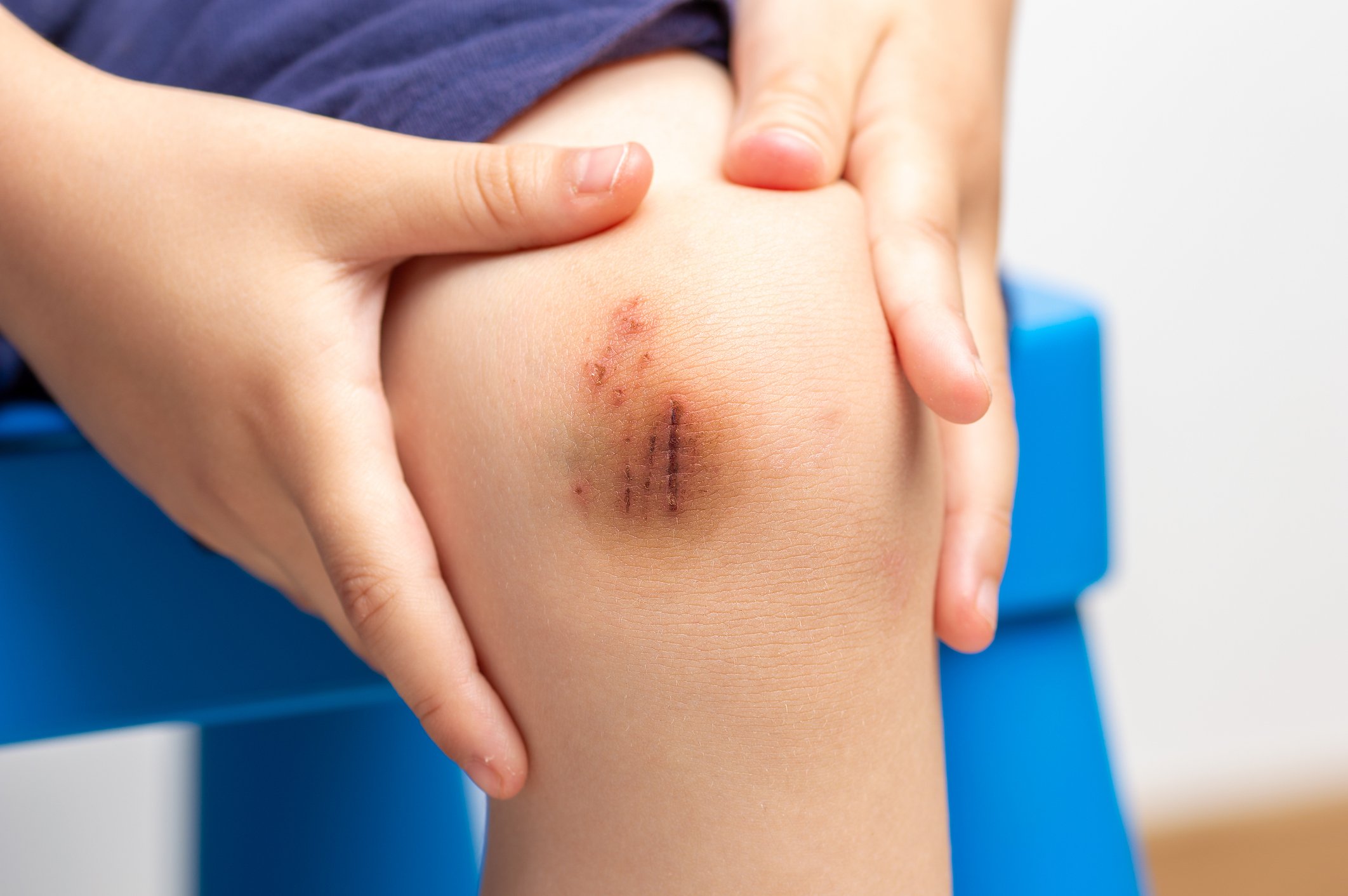
Often called a cut or a slice, a laceration is a skin tear or opening caused by injury, usually with a sharp foreign object such as a knife or glass. Lacerations, such as a paper cut, can be minor or very large. Home management may be sufficient, or emergency treatment may be necessary, depending on the severity.
For first aid for babies with a laceration, apply pressure until the bleeding stops, sometimes up to 5-10 minutes. Wash the area with soap under running water, but do not scrub. Cover the area with a bandage or gauze and keep it clean and dry.
When Does My Child Need Stitches?

Lacerations on the face that are deeper than half an inch or will not stop bleeding may require stitches.8 Reach out to your child’s pediatrician if you suspect they may need stitches.
Burns
Burns can range anywhere from mild to very severe and life-threatening. While you can manage some at home, others require immediate medical care. Call 911 immediately if your child is burned severely. Other burn situations that require medical attention include large, burned areas of skin; burns resulting from a fire, chemical exposure, or electrical wire or socket; facial, joint, hand, foot, or genital burns; or burns that appear infected with swelling, pus, or red streaking.
In the event of a burn, remove clothing from the burned area unless it sticks to the skin. Run cool water over the site until the pain subsides, then lightly apply a bandage or soft cloth. You can offer over-the-counter pain medications if your child appears to be in pain and is old enough for them. Do not apply creams or ointments, and do not break any blisters.

To prevent burns, keep babies away from space heaters, radiators, candles, irons and curling irons, hot drinks, and out of the kitchen while cooking. Always check the bath water temperature before submerging your baby. Scald burns from hot water or other liquids are the most common emergency in babies. Do your best to prevent them and be prepared if they happen.
Allergic Reactions

A typical emergency is an allergic reaction when your baby is young and introduced to new foods for the first time. Allergic reactions can range from mild to severe.
Mild allergic reactions can involve skin hives, itchy, watery eyes, sneezing, runny nose, or itchy throat. Severe allergic reactions involve multiple body systems, so look for a combination of mild symptoms. Severe allergic reactions can also cause difficulty breathing or swallowing, mouth or tongue swelling, nausea, vomiting, diarrhea, dizziness, and fainting.
If you suspect a severe allergic reaction, call 911. If you have a prescription or have access to an epinephrine auto-injector, administer it per package directions and go to the emergency room. Check with your doctor about administering an oral antihistamine medication for mild allergic symptoms. If your child receives an allergy diagnosis, they must have their emergency medications with them and ready to use at all times.9
Poisoning

If you come across your child with an open or empty bottle of a potentially toxic substance, such as a medication or cleaning supply, it is possible that they have ingested it and may be poisoned. First, remove the poison from the child’s reach in this situation. Inspect their mouth for evidence that they have eaten the substance and remove any excess from their mouth or force them to spit it out. If possible, save this for proof. Do not force your child to vomit, and do not follow the poison instructions on the package, as they may be outdated. Immediately call poison control at 1-800-222-1222 or your child’s pediatrician for instructions.10
If the poison exposure is on the skin or in the eyes, rinse the area in lukewarm water for at least 15 minutes and note any signs of chemical burning. Do not apply any ointments, creams, or butter unless your child’s care doctor or the poison control center tells you to.11
Dental

The good news about dental emergencies in babies is that you do not have to replace baby teeth. It is still a good idea to save the damaged or prematurely lost baby tooth. The mouth area may bleed and be sore, so if possible, rinse the mouth. First aid for babies with a dental emergency is to apply cold, wet gauze or ice and pressure to the site. Call your pediatric dentist to let them know what has happened, and follow any of their instructions. Keep an eye on the area for swelling, pain, or color change. You should also monitor your child for fever.12
Information on first aid for babies can be scary, intimidating, and overwhelming to read. Common emergency scenarios can be painful even to imagine, but preparing and practicing these situations is essential. Preparedness can help decrease the severity of many emergencies your child may experience. The American Red Cross and other organizations offer CPR and first aid courses that anyone can take. All parents and caregivers can benefit from this knowledge and experience.






































