One of the most common pain management options during labor is an epidural. Yet despite how frequently epidurals are used, many misconceptions still surround them. Some information shared online or passed between friends is accurate, while other claims are simply myths.
When creating your birth plan and considering your pain relief options, it’s important to understand how epidurals work, their benefits, limitations, and alternatives. Learning the facts behind common epidural myths can help you make informed decisions about your labor and delivery experience.
Key Takeaways
- Epidurals provide significant pain relief but may not completely eliminate labor pain.
- You can often change positions and labor off your back with an epidural.
- Research shows epidurals are unlikely to significantly increase your risk of C-section or assisted delivery.
- Not every laboring woman is a candidate for an epidural.
- Several alternatives to epidurals are available for labor pain relief.
What Is an Epidural?
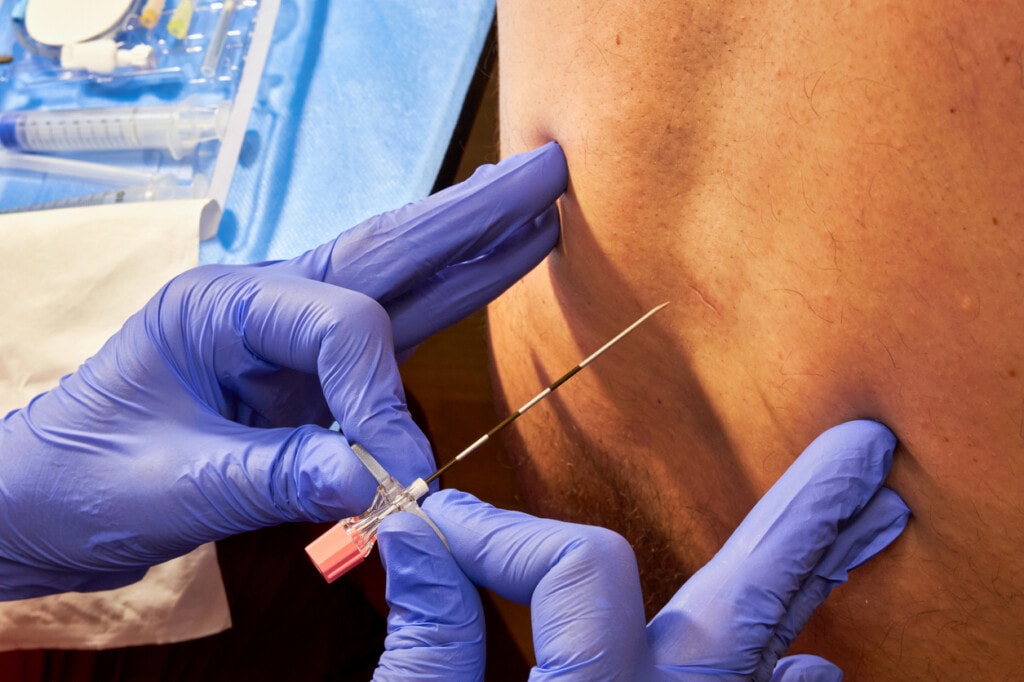
An epidural is a form of pain relief used during labor and delivery. A small catheter is placed into the epidural space near the spine, allowing medication to be delivered continuously to reduce pain while you remain awake and alert.1
Related: Epidural During Labor: Benefits, Risks, and What to Expect
Epidural Myths and Facts
Epidurals are one of the most common forms of pain relief during labor, but they are also surrounded by misconceptions. Understanding what’s true and what’s not can help you feel more confident when making decisions about your birth experience. Below, we’ll break down 10 common epidural myths and explain the facts behind each one.
Myth #1: Everyone Gets an Epidural
Epidurals do seem to be the norm these days. When a woman shares that she wants to give birth without one, she often gets crazy looks or comments about how she won’t make it. While 60 percent of American women received an epidural in 2022, that is still far from everyone.2
This statistic should not be used to coerce or pressure you into getting an epidural. What other women choose for their births does not impact what you do. Not everyone gets an epidural for birth; epidurals are not required, and they need your request and consent.
Myth #2: Epidurals Completely Relieve Your Pain
While epidurals provide good relief from labor pains, they are not guaranteed to remove all the pain of contractions. About 5 percent of the time, an epidural turns out one-sided or ineffective. Usually, in these cases, the anesthesiologist can adjust the epidural without having to redo it, but in rare cases, they may have to start over.3
If your pain control through an epidural is not adequate, the dose of pain medication administered through your epidural can be adjusted. Often, you will be given your own patient-controlled pump to give yourself a limited number of extra doses per hour.3
Most of the time, you do not want complete numbness from the pain and pressure of contractions, particularly toward the end of labor, because these sensations help you know when to push.3
Myth #3: You Can Only Be on Your Back if You Get One
Because your legs are numb and somewhat limp while you have an epidural, it is more difficult to change and hold certain positions when you have one. But with the right support, laboring in other positions is often possible. Your partner, nurse, doula, and other care team members can assist you with getting into other positions. For labor and delivery, you can also use props such as pillows, blankets, and a peanut ball to hold you in a comfortable position, such as side-lying.4
Related: Side Effects of an Epidural and What You Should Know
Myth #4: Epidurals Slow Down Labor
There is controversy in the birthing world surrounding whether epidurals slow down labor and increase the need for other interventions, such as labor augmentation with Pitocin. However, studies have shown that having an epidural does not significantly lengthen the duration of labor. It is also not likely to increase your risk for an assisted delivery with forceps or a vacuum, nor your chance for a C-section.
An epidural may, however, slightly increase the pushing phase of labor by an average of 30 but up to 50 minutes in rare cases.5,6
Myth #5: It Wears Off
An epidural will last as long as needed because it is connected to a pump that delivers continuous pain relief medication. The dose can be adjusted as needed, and the pump is usually turned off and the catheter removed after delivery. Only after the medication is turned off does the pain relief wear off.6
Myth #6: There Is a Specific Time Frame To Get One
Because an epidural lasts for as long as you need it, it is rarely too early for an epidural. If your provider has determined you are in labor and admitted you to the labor and delivery unit, you can likely request an epidural whenever needed.
If you are in late-stage labor, it may be too late for an epidural because of the time it takes to prepare for the insertion procedure. You also have to be able to sit still for the epidural insertion, which may be too difficult if you are too far along in your labor.6 With that said, our Editor in Chief has seen laboring women get an epidural at 9 centimeters dilated. If you’re able to sit still and really want an epidural, you still have the right to request one. The medical staff may discourage you because you are so close to pushing and may still need IV fluids administered, or the anesthesiologist might not be immediately available. But ultimately, it is your choice, and you can still ask.
I’ve heard stories of women who were encouraged to get an epidural earlier than needed because they might “miss their window” or the anesthesiologist is about to leave for the day. You should not be pressured into getting an epidural if you do not desire it or do not feel you need it. The only time anesthesia or pain relief is not optional is during a C-section. No one wants abdominal surgery while completely unmedicated!
Related: When To Get an Epidural During Labor
Myth #7: Anyone Can Get an Epidural
Most laboring women can indeed get an epidural. However, women with certain back or spinal issues or surgeries or with certain blood clotting or bleeding disorders may be unable to because of their increased risk factors.7,12,13 Talk to your provider about your health history and discuss alternatives if you are unable to receive an epidural but still want pain relief during labor.
Myth #8: There Are No Alternatives for Labor Pain Relief
An epidural is the most common form of pain relief for labor, but alternative pain medications exist. Some of these alternatives include opioid medications, local numbing agents, inhaled nitrous oxide, breathing techniques, and massage.8,9
A systematic review found that epidurals offered better pain relief with less need for additional pain relief when compared to opioid medications. However, alternative pain control can sometimes provide just the break a laboring woman needs before continuing with a low-intervention birth.10
Related: 32 Things Women Wish They Had Known Before Getting an Epidural
Myth #9: An Epidural Works Immediately
After requesting an epidural, it can take time for the anesthesiologist to arrive at your bedside. It also takes a few minutes to set up all the materials and prepare a sterile field in the surrounding area.
Once the doctor and the room are prepared, insertion is quick and relatively painless. Most women report that injecting the local numbing agent prior to epidural insertion is the most painful part. And after the doctor inserts the epidural catheter, it usually takes between 5 and 20 minutes to take effect.6
Myth #10: You Can’t Eat if You Get an Epidural
Many hospitals indeed restrict what you can eat and drink while in labor. If they allow food, you are typically limited to light foods such as Jell-O and applesauce, and to clear fluids like broth, juice, and ice chips. However, these restrictions do not concern whether you have an epidural. The reason is the risk of aspiration or choking if you need a Cesarean section under general anesthesia.
But even if you end up needing a C-section, it is rare to require general anesthesia. Because of advances in healthcare and new research, the no-eating-during-labor rule is slowly changing at some hospitals. Talk to your provider about whether you can eat and drink during labor, with or without an epidural.11
Related: Foods To Eat (And Not Eat) in Early Labor
Whether you choose to labor with or without an epidural, knowing the myths and facts about this pain control method will help you make an informed decision. Your birth preferences are essential; every mother deserves to feel informed, heard, and satisfied regarding her experience. Research shows that epidurals do not harm babies or prevent successful breastfeeding. Regardless of how you labor, the goal is the same: welcoming your baby into the world.6