A cleft lip or cleft palate is a congenital anomaly defined as a “group of disorders affecting the structure of the face and oral cavity.” A baby can be born with a cleft lip, a cleft palate, or both. When babies are born with either, they need extra special attention to help meet their needs.2 Various factors can cause a cleft palate or a cleft lip. The diagnosis of either puts a child at a higher risk for concerns related to feeding, nutrition, hearing, and facial, orthodontic, and dental abnormalities. A multidisciplinary healthcare team can help address these concerns and assist the family in navigating care for their child.1
What Are a Cleft Lip and a Cleft Palate?
A cleft lip occurs when the infant’s lip does not fuse completely together. The baby is then born with a separation in the lip. A cleft palate occurs when the baby’s palate does not completely fuse, causing the baby to be born with a gap or opening in the roof of the mouth.4,5 There are various degrees in which a cleft lip or cleft palate can occur. Diagnosis can be unilateral, occurring on one side, or bilateral, shown on both sides.4,5
What Causes a Cleft Lip or Cleft Palate?
So, what causes a cleft lip, and what causes a cleft palate? Although what causes a cleft lip and palate is unknown, many are thought to be a result of gene mutations or a mother’s exposure to environmental factors during pregnancy. The Centers for Disease Control and Prevention (CDC) has found that maternal smoking, diabetes, and using certain medications increase the risk of their baby developing a cleft lip or cleft palate.6 Let’s explore how diagnosis and treatment work for these disorders:
Diagnosis
Most parents find out their baby will be born with a cleft lip early since it can be diagnosed through ultrasound. A cleft palate, on the other hand, can be diagnosed early but is not as commonly diagnosed by ultrasound and is usually noticed quickly after birth. The pediatrician plays a vital role in the early diagnosis of a cleft palate not diagnosed prenatally. Some babies may not even be diagnosed until later when they are not gaining weight appropriately or have feeding difficulties. The child is usually diagnosed with a submucosal cleft palate in these circumstances.2,3,7
Treatment
Care coordination is extremely important when treating a child with a cleft lip or cleft palate due to the child’s complex medical needs. A specialized healthcare team with a multidisciplinary approach can often cover every need. A typical team usually includes pediatrics, dentistry, orthodontics, plastic surgery, audiology, genetics, oral surgery, and otolaryngology. It can also be helpful to involve speech pathology, psychology, nutrition, and social work in the care team. Care plans should be specialized to each child and focused on their needs.11,12
Surgery to correct the cleft lip or cleft palate will be based on each child and sometimes will occur in stages. Cleft lip repair surgery usually occurs between 3 to 6 months old. This repair is known as a cheiloplasty. Cleft palate repairs, also known as palatoplasty, close the gap between the nasal and oral cavities. The palatal musculature is also reconstructed during this procedure to enable normal speech development. The cleft palate repair is commonly done between 9 and 18 months old. Following the initial procedures, follow-up surgeries may be needed or recommended to assist with speech and the appearance of the lip and nose area of the child.2,8
Surgery is a large part of the child’s treatment plan, but even before and after surgery, many other healthcare disciplines will play a role in meeting the child’s medical needs.
Feeding a Baby With a Cleft Lip or Cleft Palate
It is essential to find the best feeding method for your baby and continually educate yourself on how to support your little one best. As you explore different ways of feeding your little one, it is essential to monitor their weight gain, making sure the method is appropriate. Below, we will explore three feeding methods and how to best approach them for a baby with a cleft lip or cleft palate:7
1. Breastfeeding
A key component for successful breastfeeding is creating suction. Suction helps the baby latch and stay on the breast to suck and trigger the mother’s letdown, and the movement of the baby’s tongue helps transfer milk from the breast. This becomes a more complex problem for a baby with a cleft lip or palate.7 Some babies with a cleft lip or palate may appear to latch but are more commonly seen as “chomping” and cannot transfer milk and swallow appropriately.5
Challenges differ between children depending on the variation of cleft they have. It is more common for babies with a cleft lip to have better success breastfeeding than a child with a cleft palate or both.7
Tips for Breastfeeding a Baby With a Cleft Lip or Palate
Here are some tips from the Academy of Breastfeeding Medicine regarding breastfeeding a baby with a cleft lip or palate:5,7
- After cleft repair, breastfeeding can resume right away.
- Even if the baby cannot remove milk effectively from the breast, putting your baby on your breast can help with bonding and comfort for the baby.
- A lactation specialist can assist with, evaluate, and discuss the possibility of breastfeeding and offer education about milk supply and expression.
- Draw your baby tightly to the breast and use your thumb over the cleft lip area to help close the area, creating a seal for your baby to breastfeed.
- If unable to breastfeed, it is essential to express milk with a breast pump to maintain your breast milk supply.
2. Bottle Feeding
It is common for babies with a cleft lip or cleft palate to need a special feeding device. Just as with breastfeeding, when sucking a bottle, it is challenging to create suction to remove milk. You can try a variety of special bottles and nipples to find the best fit. You can work with a feeding specialist to find the right device for your baby. Some of these special and supportive feeding devices include Dr. Brown’s Specialty Feeding System, the Haberman Feeder, Pigeon Cleft Palate, and Mead-Johnson Cleft Lip/Palate Nurser.2
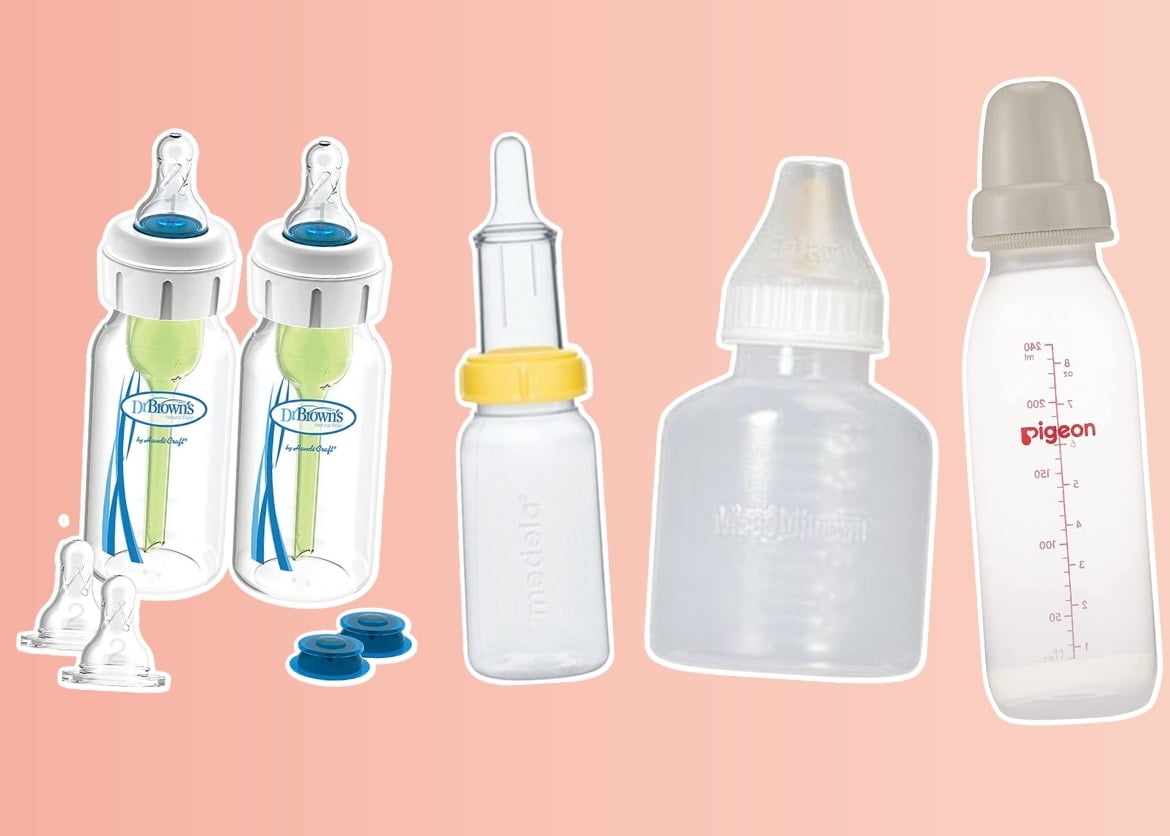
Even when using a special feeding device, feeding strategies and techniques may help your little one successfully and comfortably feed.
Bottle Feeding Tips for Feeding a Baby With a Cleft Lip or Cleft Palate
Here are some tips on bottle feeding your baby if they have a cleft lip or cleft palate:
- Feed in the upright position to help decrease nasopharyngeal reflux.
- Use the “dancer-hand” feeding position. This position supports the baby’s lip, chin, and cheeks to help with sucking movements.
- Take feedings slowly. Allow the child to take breaks to breathe.
- Synchronize “squeezing” milk to the child from the bottle with their sucking pattern.
3. Feeding Solid Foods to a Baby With a Cleft Lip or Palate
Just as with children without a cleft lip or cleft palate, you can introduce solid foods around 6 months. You should watch for signs your child is ready to start solids. These include holding their head up on their own, sitting upright with minimal support, and showing interest when others eat. If you are unsure your child is ready, speak with their healthcare team. Children with a cleft palate may experience food entering their noses while eating. This can be alarming and very uncomfortable for the child. The child can usually clear the food by sneezing or drinking.10
To help the child handle the food in their mouth easier, children with a cleft palate need to start with thicker purees with no clumps. As your child grows comfortable with the purees, you can slowly add more textures with other soft foods. It’s helpful to work with your healthcare team and a feeding specialist for guidance on feeding your little one solid foods.10
The Bottom Line
Children born with a cleft lip or cleft palate need extra support and care from the start. With an excellent healthcare team on hand, you can navigate your child’s healthcare needs. It is important to contact your health care team if you notice any concerning or new changes, your little one is not feeding well, you feel they are losing weight, or any questions arise.





































