Pregnant moms often worry about all that can go wrong during pregnancy, labor, and delivery. You might want to know all the possibilities so you can prevent them. One thing you may have heard about is a nuchal cord. Stories circulating online tell of pregnant moms sent to hospitals after getting a sneak peek or a boutique ultrasound, and the technician thinks the cord is around the baby’s neck.
It’s scary to imagine the umbilical cord wrapping around a baby’s neck during pregnancy! Images of your yet-to-be-born baby suffocating from their cord might haunt you. However, your baby not only gets nutrition through their cord but also oxygen that way, not through breathing. Here, we’ll look at the truth about nuchal cords — what they are, who’s at risk, and when to worry.
What Is the Umbilical Cord?
The umbilical cord (sometimes called a baby’s lifeline) connects the mother’s placenta to the baby’s circulation. It supplies blood, nutrients, and oxygen to the fetus while removing waste. It typically consists of three blood vessels — two arteries and one vein — surrounded by a gelatinous substance called Wharton’s jelly and an outer coating like a thick skin holding it all together.1
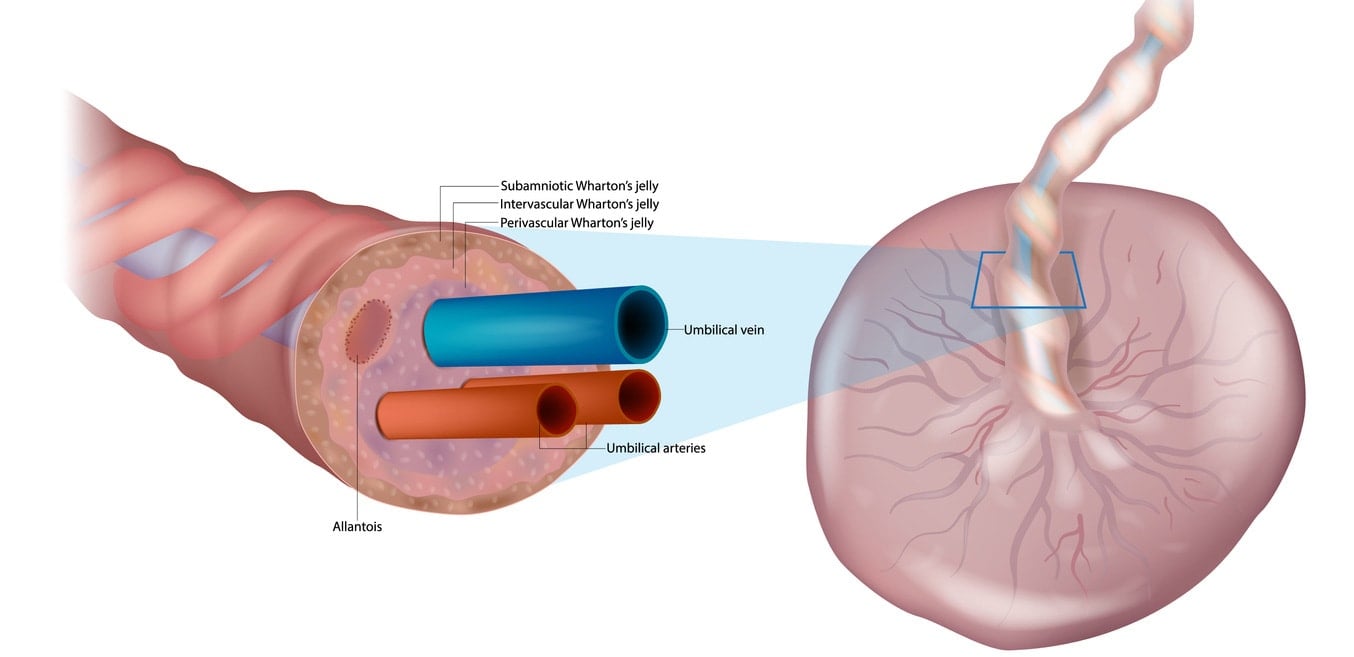
Wharton’s jelly helps insulate and protect the umbilical blood vessels from compression or constriction due to loops, knots, kinks, fetal grasping, and labor contractions. This insulation and protection help maintain adequate blood flow to and from the baby during pregnancy despite the surrounding environment and circumstances. The umbilical cord can protect itself and maintain its function.2
What Is a Nuchal Cord?
The umbilical cord can become wrapped 360 degrees around a baby’s neck during pregnancy.2 This is a nuchal cord, as “nuchal” refers to the neck.9 The cord can wrap just once or multiple times around and be tightly or loosely wrapped.2,8
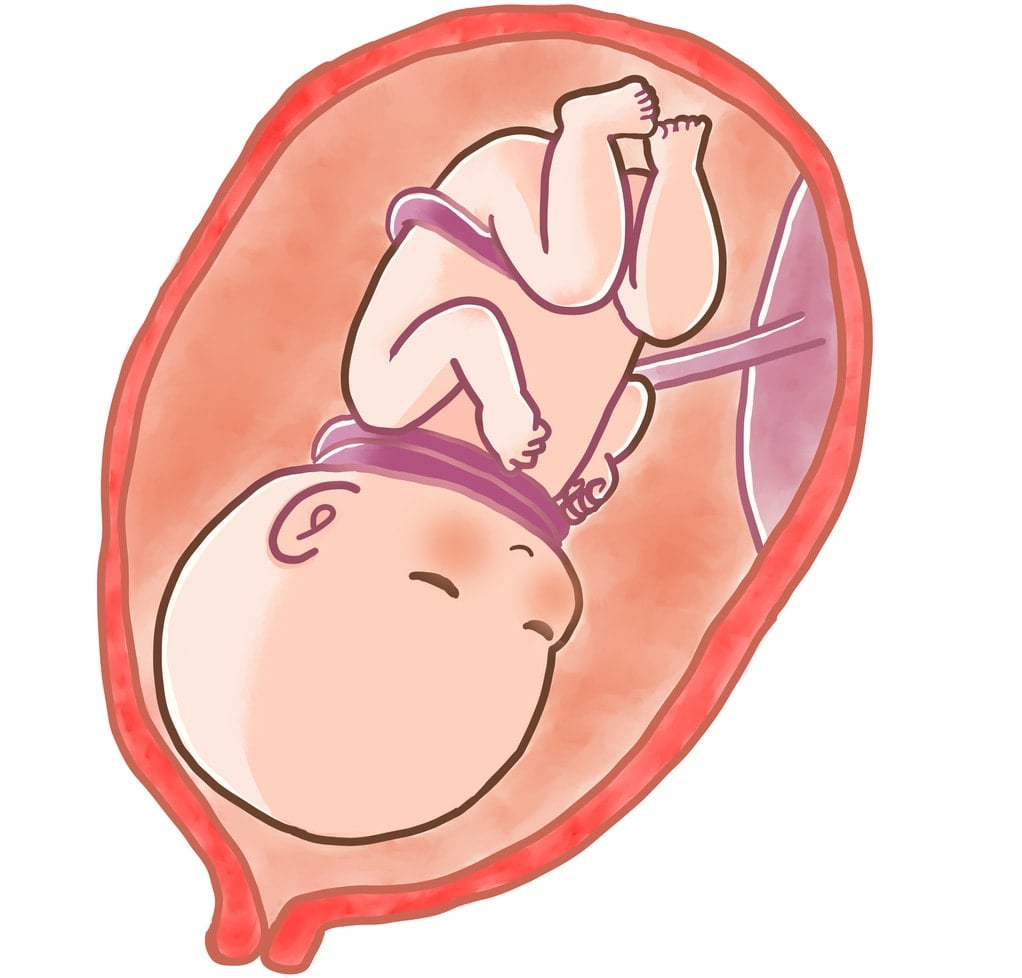
Researchers have identified two formations of nuchal cords — unlocked and locked — depending on the orientation of each end of the cord. Unlocked cords slide freely and can often unwrap themselves. Locked cords are much less likely to come undone on their own. And if they do, they will likely form a true knot in the umbilical cord.2
What Are the Risk Factors?
A nuchal cord happens because of random fetal movements that allow the cord to end up wrapped around the neck. Excess amniotic fluid allows for more fetal movement, which can increase the risk of a nuchal cord.3 Extra-long umbilical cords greater than 27.5 inches also allow for more slack and more likelihood of cord entanglement. For reference, the average cord length is 21 inches.3,4
Other circumstances in pregnancy can lead to a higher prevalence, including:4
- Marginal cord insertion (when the umbilical cord originates from the edge of the placenta instead of from the center)
- Pregnancy duration of more than 42 weeks
- Male fetus
How Common Is a Nuchal Cord?
They’re common and occur in about 10%-29% of fetuses, with an overall incidence of 6% at 20 weeks and 29% at 42 weeks.2
What Are the Risks of Having a Nuchal Cord?
A nuchal cord can increase the risk of other conditions at birth, especially if the cord is wrapped tightly or multiple times. However, it usually doesn’t increase the risk of adverse birth outcomes.5
One study showed a slight association between nuchal cords and meconium staining. Meconium staining is when a baby has their first bowel movement in utero before delivery, which can sometimes put them at risk for respiratory difficulties after birth. However, this association was in post-term pregnancies in which the baby had multiple loops in the cord.5
If a nuchal cord causes the cord to become compressed, it can restrict blood flow through the cord, especially during contractions. This may cause a temporary decrease in fetal heart rate, called deceleration, which would show up on fetal heart rate monitoring during labor. A stillbirth could occur if something cuts off cord blood flow for long enough.2
Studies haven’t demonstrated an increased risk of stillbirth due to the presence of a nuchal cord, mainly when accounting for confounding risks such as diabetes, high blood pressure, premature rupture of membranes, low amniotic fluid, and fetal anomalies.6 Nuchal cords also didn’t increase a mom or baby’s risk for:6
- C-section
- Instrumental delivery for fetal distress, such as the use of forceps or vacuum
- Low APGAR score
When Is a Nuchal Cord Diagnosed?
A doctor will often detect the presence of a nuchal cord via ultrasound, but it’s considered an incidental finding. An incidental finding is something discovered in a test performed for an unrelated reason. There’s also a relatively high false-positive rate of 20% for a nuchal cord when diagnosed via ultrasound. This is because you don’t always get multiple or three-dimensional views. A false positive means an ultrasound can often show a nuchal cord that isn’t there. For instance, perhaps the cord is just crossing the baby’s neck but not wrapped all the way around.5,6 Color imaging can aid in the diagnosis of a nuchal cord via ultrasound. This imaging shows the speed and direction of blood flow, which helps to visualize if the cord wraps all the way around.6,7
Your obstetrician may also do a test for a nuchal cord in which they manually compress the fetal neck through your abdomen. If this causes the fetal heart rate to drop, the test is considered positive for the presence of a nuchal cord.2 Nuchal cords are suspected in labor if continuous fetal heart rate monitoring reveals variable decelerations. This means the baby’s heart rate drops at different or seemingly random times during contractions.5
Although nuchal cords can be suspected using ultrasounds, doppler imaging, and various tests and signs during pregnancy and labor, they can only be definitively diagnosed at delivery. So, you cannot know your baby has a nuchal cord until their head is out.6
What Should You Do if You Have a Nuchal Cord?
There’s no way to untangle it before delivery intentionally. Just as random fetal movements can cause the cord to tangle, random movements may cause some nuchal cords to untangle on their own. However, it’s very rare for a nuchal cord to untangle itself after labor begins.2 Here’s what to do if you have one:
Attend Prenatal Appointments
If your doctor has diagnosed you with a nuchal cord, attend all your prenatal appointments to monitor the baby’s heart rate as well as your weight and blood pressure, particularly as labor approaches.
Monitor Fetal Heart Rate Intermittently
Sometimes, moms opt for intermittent fetal heart rate monitoring because it allows them to be more mobile. Intermittent monitoring is when you’re hooked up to a monitor for 20 minutes each hour. However, suppose your provider suspects a nuchal cord. In that case, you may consider continuous fetal heart rate monitoring to look for signs of cord compression, like variable decelerations.2
Routine Check at Delivery
Because a nuchal cord often isn’t diagnosed until delivery, your provider will routinely check for it once the baby’s head is delivered. If the umbilical cord is wrapped loosely around the baby’s neck at delivery, your provider gently slips it off the head. If it’s too tight to do so, they’ll clamp and cut the cord before delivering the baby’s shoulders to prevent the cord from tearing away from the placenta, which could cause a hemorrhage or excessive bleeding.3
The Bottom Line
Since the possibility of adverse effects is low, try not to worry about a nuchal cord.8 Communicate any concerns to a provider whose judgment you trust, and advocate for the birth you want. For example, don’t allow anyone to pressure you into a C-section because of a nuchal cord alone. Know the facts!
It can be scary to learn that your baby may have their umbilical cord wrapped around their neck. But it most often means nothing for your birth plan or your baby’s future health. Nuchal cords are common, and as hard as it may be, try not to panic if you think you may have one.2 Your providers are familiar with and prepared to handle them without adverse effects.