If you have young children, especially those in daycare or preschool, it can feel like illnesses spread nonstop. One common childhood illness many parents eventually encounter is hand, foot, and mouth disease (HFMD), a contagious viral infection most often seen in children under 5.
HFMD can cause fever, painful mouth sores, rash, irritability, and decreased appetite, making little ones feel pretty miserable for several days.1,2 While the illness is usually mild and resolves on its own, understanding the symptoms, how it spreads, and when to contact your pediatrician can help parents feel more prepared.
Here’s what parents should know about hand, foot, and mouth disease.
Fortunately, most cases are mild and improve with rest, hydration, and supportive care at home.
Key Takeaways
- Hand, foot, and mouth disease is a common viral illness in young children.
- Symptoms often include fever, mouth sores, rash, and irritability.
- HFMD usually resolves on its own within 7 to 10 days.
- Hydration, rest, and symptom management are the most important parts of care.
- Contact your pediatrician if symptoms worsen or your child shows signs of dehydration.
What Is Hand, Foot, and Mouth Disease?
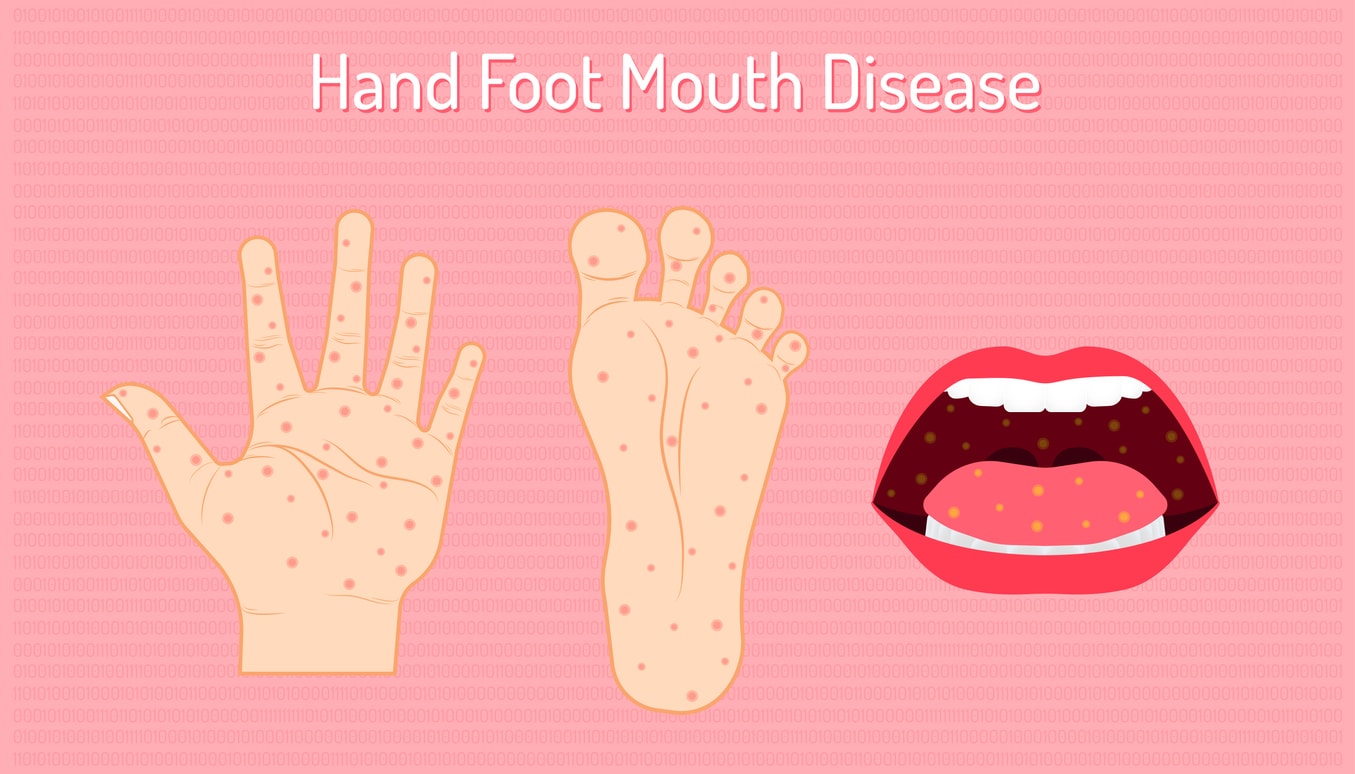
Hand, foot, and mouth disease (HFMD) is viral, but various viruses can cause it. Typically, an enterovirus such as coxsackievirus causes HFMD. Although sometimes confused for each other, hand, foot, and mouth disease is not the same as foot-and-mouth disease that animals sometimes get. HFMD cannot be given to or acquired from animals.2 When a person’s symptoms match the description, regardless of the specific viral cause, it would be diagnosed as hand, foot, and mouth disease.2
Related: The Best Ways To Treat a Baby’s Cold
Symptoms of Hand, Foot, and Mouth Disease
Symptoms of HFMD can vary slightly from child to child, but the illness often follows a recognizable pattern.
At the start of the illness, symptoms may resemble those of a common cold, including a runny nose, a sore throat, a headache, and a fever.3 As the disease progresses, you may see symptoms more unique to hand, foot, and mouth disease. These include mouth sores and a rash on the palms of the hands and the soles of the feet. The red spots in the mouth, hands, and feet are typically flat, not raised. The sores may eventually blister, but typically do not burst. Sometimes, a rash in the diaper area can occur.4,5,6
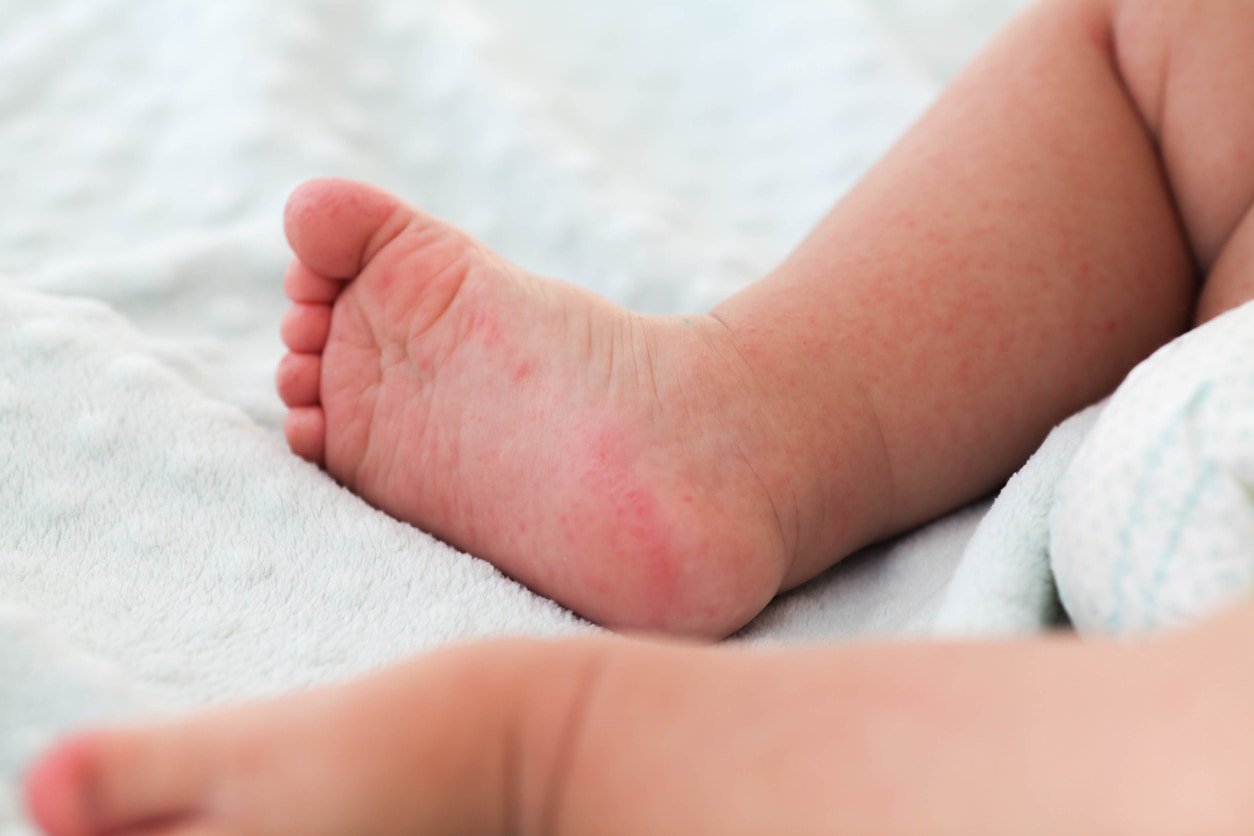
Getting a good look inside your child’s mouth can sometimes be challenging. Some signs that they may have painful sores in the mouth include not eating or drinking, or only wanting to drink very cold liquids. Children with painful mouth sores may drink less than usual, increasing the risk of dehydration. You may also notice excessive drooling, which can mean that swallowing is painful.4
Related: What to Know About Dehydration in Babies
How Long Does Hand, Foot, and Mouth Disease Last?
After exposure to the virus, it may take three to six days for the symptoms of HFMD to appear. This is called the incubation period. Most symptoms improve within 7 to 10 days, with 2 or 3 days of fever followed by a rash lasting up to a week. However, symptoms should not be at their peak for this long.1,6
The CDC recommends contacting your child’s pediatrician if their fever lasts more than 3 days or their symptoms last longer than 1 week. They also recommend contacting a provider if your child is under 6 months old, has a weakened immune system, or refuses to drink.4
How Hand, Foot, and Mouth Disease Spreads
HFMD spreads easily among young children, especially in group settings like daycares and schools.
Hand, foot, and mouth disease is spread through respiratory droplets. Anyone who comes into contact with an infected person’s mucus or saliva, including drool, may become sick. It can also be transmitted through stool, such as when changing a diaper.2
The most important thing you can do to prevent the spread of HFMD is to wash your hands frequently. It is also essential to disinfect high-touch surfaces and toys. Avoid touching your eyes, nose, and mouth, and keep your distance from people who are sick.1
Children are often most contagious during the first week of illness, but the virus can sometimes remain in the body longer.
Managing Symptoms of Hand, Foot, and Mouth Disease
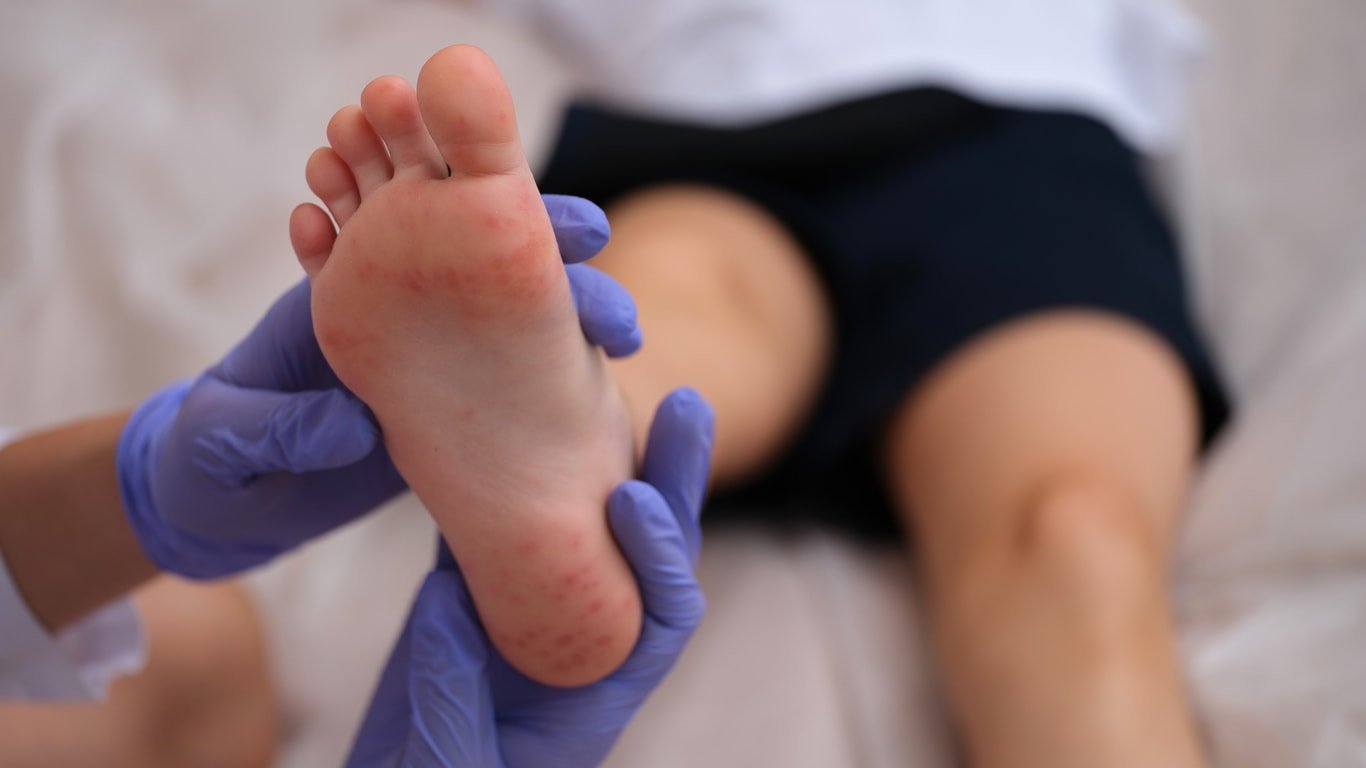
Because HFMD is caused by a virus, treatment focuses mainly on managing symptoms and keeping children hydrated and comfortable while the illness runs its course.1,5
Fever
If your child is experiencing discomfort due to a fever, you can consider giving ibuprofen or acetaminophen to lower their temperature. Refer to the package instructions and your pediatrician for appropriate dosages. However, if the fever is less than 102 degrees Fahrenheit, it may be beneficial not to treat it, as this helps fight the infection.7 As with any fever, ensuring your child stays hydrated is vital. Encouraging fluids is important to help prevent dehydration during illness.
Related: Fever in Babies: A Parent’s Guide and Treatment Tips
Pain
Ibuprofen or acetaminophen can also help alleviate pain associated with the sores on the hands, feet, and mouth.
Oral Pain
A pediatrician may recommend certain supportive measures, such as liquid antacids, to help reduce discomfort from oral blisters. In children older than one, these may sometimes be applied carefully inside the mouth with a cotton swab. Older children may be instructed to swish and spit small amounts as directed by their healthcare provider. Alcohol-based mouthwashes should not be used because they may increase pain.
Children with mouth sores may tolerate cold liquids and softer foods more easily during the illness. Maintaining fluid intake is especially important while recovering from HFMD.
Related: How To Soothe Hand, Foot, and Mouth Disease at Home
Possible Complications of HFMD
While no illness is fun, HFMD is often mild and short-lived. Rare complications of hand, foot, and mouth disease include fingernail and toenail loss, viral meningitis, and brain swelling. Long-term effects are exceedingly rare. Most children recover fully after several uncomfortable days at home.
If your child has a fever, is excessively drooling, or seems unable to keep up with normal school activities, you should keep them home. Otherwise, the CDC says they can continue to attend.2
Hearing that hand, foot, and mouth disease is circulating in your child’s classroom or daycare is never fun for parents. Fortunately, most cases are mild and improve within about a week with rest, hydration, and symptom management.
If your child develops worsening symptoms, signs of dehydration, persistent fever, or difficulty drinking fluids, contact your pediatrician for guidance. While HFMD can make children uncomfortable for several days, long-term complications are uncommon.