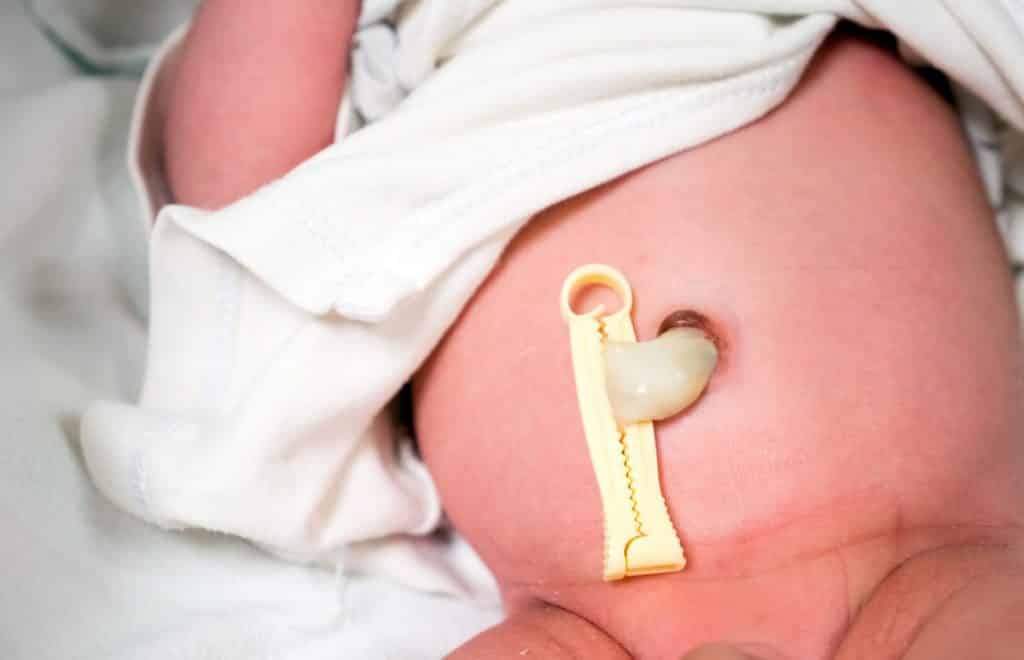
Until recently, medical staff have been discarding the placenta and umbilical cord as medical waste after babies were born.2 Now, research shows us that there are multiple therapeutic uses for cord blood — the blood that remains in a baby’s placenta and umbilical cord after the delivery of the baby and the cutting of the umbilical cord — and now even cord tissue.3 But why would someone want to save their baby’s cord blood or cord tissue? Here, we’ll explore cord blood banking vs. cord tissue banking and why parents might do it.
What Can Cord Blood or Tissue Be Used For?
Cord blood contains a rich source of blood-forming cells known as hematopoietic stem cells (HSCs).1 It’s also a source of regulatory T-cells, which are immune cells.4 These are important in controlling the immune system and may have therapeutic potential in treating immune disorders.5 Cord blood stem cells have been successfully used for over 20 years to treat children and adults for more than 80 diseases and conditions. These include leukemias, lymphomas, myeloma, other serious blood disorders, and some solid tumors.1,6
Cord tissue contains groups of cells not generally found in cord blood. It’s a rich source of mesenchymal stem cells (MSCs).1 In laboratory studies, researchers have shown that these cells can form a variety of cells. These include muscle cells, bone, cartilage and tendon, skin cells, and even nerve cells.1,7 It’s the subject of over 300 clinical trials and, in the future, can hopefully treat conditions like:1
- Heart disease
- Type 1 diabetes
- Lung cancer
- Parkinson’s disease
- Crohn’s disease
- Multiple sclerosis
- Spinal, brain, and cartilage injuries
This research is still at an early stage and medical treatments aren’t currently available. However, the unique properties of these cells make them promising for future cellular therapies.
How Much Does All of This Cost?
More and more expectant parents are understanding the value of preserving stem cells from not only the cord blood but also the cord tissue and placenta tissue of their newborn baby. With this increase in interest, parents are, of course, focusing on how much bank they’re getting for their buck.
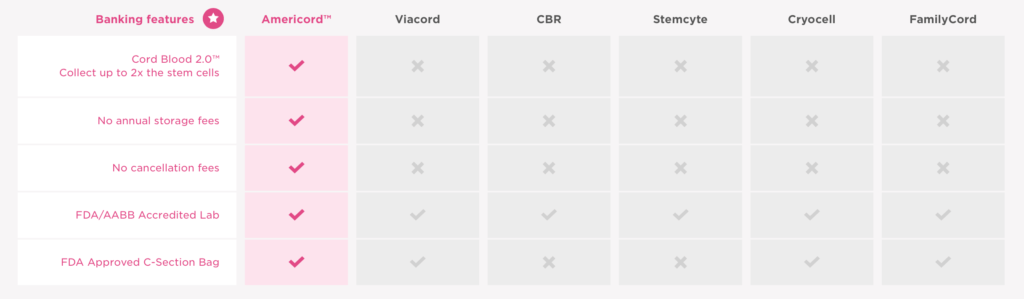
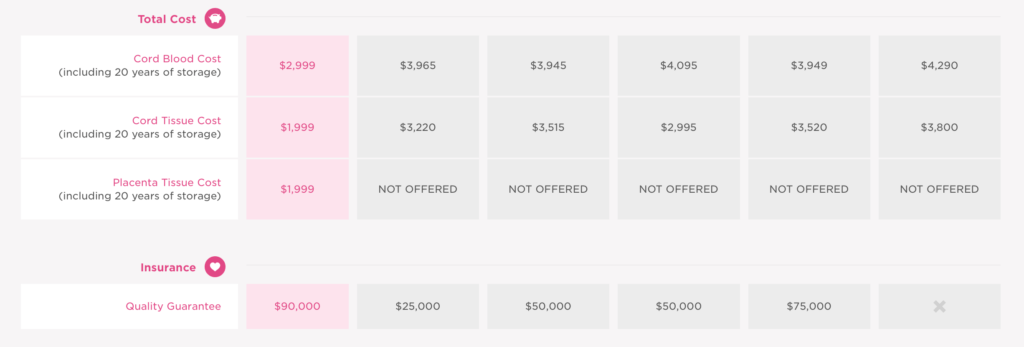
Americord recognizes this and is offering affordable prices to all new parents. They’re now being recognized by expectant parents whose budgets don’t stretch to the prices charged by top competitors. Not only that, Americord is making headlines by offering attractive, affordable options to preserve stem cells from all three available sources — cord blood, cord tissue, and placenta tissue.
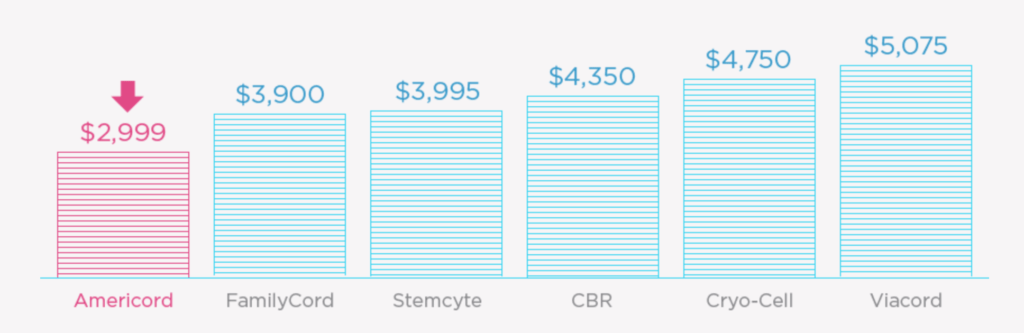
For a better idea, look below at the competitors’ prices compared to the value delivered. What’s great is that for the essential plan, Americord charges less than $4,000 for cord blood and cord tissue banking, plus 20 years of storage. That’s a deal you can’t find anywhere else.

“We believe strongly in the value of preserving as many stem cells as possible from every available source when a baby is born,” said Americord CEO Martin Smithmyer. “Our commitment to delivering the highest quality services at the lowest possible price is making it possible for more expectant parents to preserve more of their baby’s stem cells than they can with any other cord blood bank.”
To Bank or Not To Bank?
Many parents are nervous to bite the bullet and pay for banking their baby’s cord blood or cord tissue. This is because they aren’t sure if they’ll ever need these stem cells. Although it’s difficult to estimate the likelihood of using stem cells, some published studies have estimated the chance of needing a stem cell transplant from any source (i.e., cord blood, etc.) to be the following:
- The chance of a child (ages 0 to 21) needing therapy using their own stem cells is currently about 1 in 2,700.8,9
- The chance of an individual needing stem cells (either their own or from someone else) for transplantation over the course of their lifetime is estimated to be about 1 in 217 (ages 0 to 70).10
These estimates don’t include future therapies that may develop over time. While the probability of a child needing a transplant (e.g., for leukemia) in early childhood is likely low, the emerging regenerative medicine technologies and clinical trials taking place support parents in researching their options for the future.
Ultimately, the choice of banking these precious stem cells belongs to the parents. If you’re thinking about collecting your baby’s cord blood or cord tissue, talk to your obstetrician or midwife for more information. And be sure to do your own research, too.